Prostat Kanseri Nedir?
Prostat kanseri, erkeklerde en sık görülen kanser türüdür. Kansere bağlı ölümlerde ise ikinci sırada yer alır. Prostat, erkeklerde bulunan, yaklaşık olarak bir ceviz büyüklüğünde, mesanenin altında yerleşmiş, üreme faaliyetleri için çeşitli salgılar üreten bir salgı organıdır. Prostat kanseri, prostat dokusunu oluşturan bazı hücrelerin anormal seyir göstererek tümör yapıları oluşturması sonucu meydana gelir. Kanserler, prostatın sadece bir kısmından gelişebileceği gibi birden çok kısmında da gelişebilir.Genellikle 65 yaş üstünde görülen bu hastalık erken dönemlerinde hiçbir belirti vermeyebilir. Fakat tedavi edilmezse zamanla büyüyerek idrar kanalına baskı yaratabilir. Böyle hastalarda idrar yapmayla ilgili bazı şikayetler meydana gelir.
Tanı ve tedavide geç kalınmış bazı hastalarda kanserli dokular prostat içinde sınırlı kalmayıp etraf dokulara yayılım gösterebilir.
Prostat Kanseri Nedenleri Nelerdir?
Prostat kanserinde en önemli risk faktörleri yaş ve aile öyküsüdür.Yaş
Prostat kanserinin yaş ile görülme sıklığı artar. 70 yaş üzeri erkeklerin %50’sinde, 90 yaş üzerindekilerin de hemen hemen hepsinde mikroskobik düzeyde prostat kanseri tespit edilmektedir. Hastalığa 50 yaşından genç bireylerde sık rastlanmıyor.
Bu nedenle, erken teşhis için 50 yaşın üstündeki erkeklere prostat kanseri taraması öneriliyor.
Aile Öyküsü
Yapılan çalışmalar hastaların yaklaşık % 15’lik bir bölümünde diğer aile üyelerinin de prostat kanseri öyküsü olduğunu ortaya koymuştur. Prostat kanserinin oluşmasından sorumlu kimi gen grupları tanımlanmıştır.
Bunların yanı sıra, obezite ve sigara kullanımı da prostat kanseri için tanımlanan risk faktörleri arasındadır.
Prostat Kanseri Belirtileri
Lokalize (prostata sınırlı) prostat kanseri sıklıkla hiçbir belirti vermeden gelişir. Prostat kanserinin izlenebilir belirtileri şunlardır:- Özellikle geceleri sık idrar çıkma ihtiyacı
- İdrar yapmaya başlarken ya da durdururken zorlanma
- Damla damla, kesintili idrar yapmak
- Cinsel ilişki sırasında ve boşalma anında ağrı, yanma, acı hissetmek
- Cinsel ilişki sonrası boşalma miktarında azalma
- İdrarda ya da menide kan görülmesi
- Ereksiyon sırasında zorlanma
Bu belirtiler prostat kanserinin ileri evrelerinde de izlenebilir. Prostat kanseri erken evrelerinde bu semptomları göstermeyebilir. Prostat kanserinin tanı ve tedavisinin gecikmesi, kanserin komşu organ ve dokulara yayılmasına neden olabilir. Yakın lenf düğümleri, kemikler ve komşu organlarda tutulum görülebilir. Kanserden etkilenen doku ve organlarda, bulunduğu bölgeye bağlı semptomlar gelişebilir.
Prostat Kanseri Nasıl Teşhis Edilir?
Günümüzde sağlıklı bir erkeğin prostat kanseri olacağını ortaya koyan bir erken tanı yöntemi yoktur.
Artan yaş ve genetik yatkınlık prostat kanserinde ortaya koyulmuş risk faktörleridir. Bu risk faktörlerinin ışığında hastalara erken tanı amaçlı testler yapılmaktadır.
Ailesinde prostat kanseri öyküsü olmayan erkeklerde prostat kanseri taraması 50 yaş ve sonrasında tavsiye edilirken, ailesinde prostat kanseri öyküsü olanlarda daha erken yaşlarda prostat kanseri için tarama tavsiye edilmektedir.
Tarama amaçlı olarak kullanılan yöntemler parmakla rektal muayene (prostata yönelik) ve kan testi ile PSA ölçümüdür.
Kanserin Tanısında PSA Testi ve Prostat Muayenesi
Kan örneğiyle bakılan PSA (prostat spesifik antijen) testi ile prostat kanseri erken teşhis edilebilir. Prostat kanserinin erken teşhisi, tedavi olanaklarının artması açısından önemlidir.
PSA, kanser dışında bengin prostat hiperplazisi – BPH (prostat büyümesi), prostatit (prostat iltihabı), cinsel ilişki, biyopsi, rektal prostat muayenesi, idrar yolu enfeksiyonu, idrar yolu girişimleri (sonda takmak) ve ameliyatları sonrasında yüksek çıkabilir.
Bu sebeple PSA’nın yüksekliği kanser olduğu anlamına gelmediği gibi düşüklüğü de kanseri ekarte etmek için yetersiz kalabilir. Bu sebeple prostat kanserinin taraması ve teşhisinde PSA testi, prostat muayenesi ile desteklenebilir. Bu tetkikler sonucu prostat kanserinden şüphelenilen hastalara prostat kanserinin teşhisi için bazı ilave tetkikler yapılabilir:
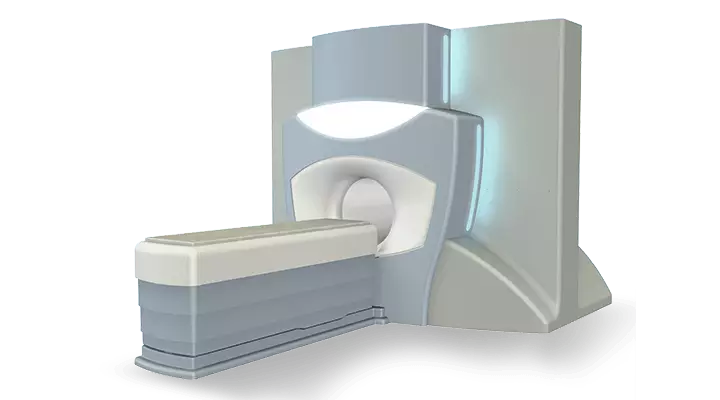
Multiparametrik MR
Prostat kanseri şüphesi olan hastalarda tanıyı destekleyebilecek bir görüntüleme yöntemidir. Kanserli olan hücre ve dokular hücre yoğunluğundaki artış ve kanlanma gibi kimi özellikleriyle sağlıklı olan dokulardan farklı bir görüntüye sahiptir. Bu sayede multiparametrik MR ile görüntülenmeleri mümkündür.
Bunun yanı sıra, Multiparametrik MR ile tümörün prostat kapsülünü aşıp aşmadığı ve olası lenf nodu sıçramaları tespit edilebilir. Ayrıca bu MR görüntüleri hastaya prostat biyopsisi yapılırken kılavuz olarak da kullanılabilir.
Prostat Biyopsisi
Mikroskop altında incelemek ve çeşitli testler yapmak amacıyla, vücudun herhangi bir kısmından doku ya da hücre parçası alınması işlemine biyopsi denir.
Prostat biyopsisinde de prostatın farklı bölgelerinden örnekler alınır. Standart prostat biyopsisinde, lokal anestezi altında rektuma yerleştirilen özel bir cihaz yardımıyla prostattan rastgele parçalar alınır. Daha sonra, patolojik incelemelerde bu dokular içinde kanserli hücre olup olmadığına bakılır.
Teknolojinin gelişmesiyle yeni biyopsi yöntemleri geliştirilmiş bu sayede tanı doğruluk oranları arttırılmıştır. Prostat biyopsisi prostat kanseri teşhisi koymada ve tümörün hızlı ve agresif seyredip seyretmediğini belirlemede kullanılır.
Standart Prostat Biyopsisi
Prostat biyopsisi makat yolu ile özel bir ultrason eşliğinde, otomatik biyopsi iğneleri ile yapılıyor. Bu şekilde yapılan biyopsi işlemleri genelde lokal anestezi eşliğinde yapılıyor ve herhangi bir yatış gerektirmiyor.
Bu işlem esnasında ultrason kılavuzluğu, biyopsinin istenilen bölgelerden alınmasını sağlıyor. PSA yüksekliğinin sebebi aydınlatılamazsa, PSA yükselmeye devam ederse veya prostat biyopsisi sonucu şüpheli olursa biyopsiyi tekrar etmek gerekebiliyor.
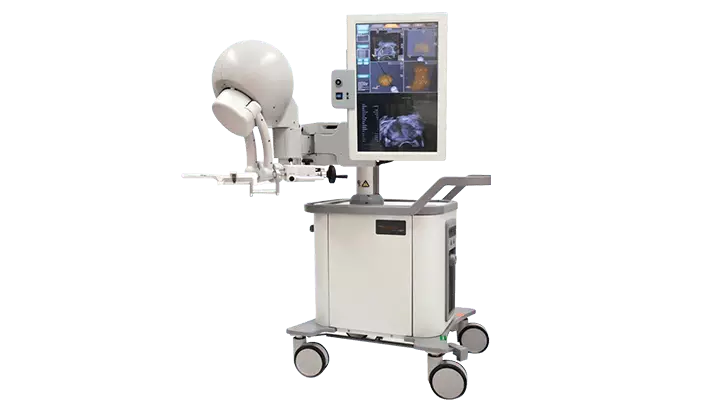
MR-Ultrason Füzyon Biyopsi
Bu yöntemde hastanın daha önce çekilen multiparametrik MR görüntüleri, prostat biyopsisi yapılan ultrason cihazına aktarılarak tümörün tam yeri belirlenebilmektedir.
Böylelikle klasik biyopsilerdeki gibi “rastgele” parça almak yerine “hedef gözeterek” direk şüpheli odaktan biyopsi yapılır. Tümörün ya da şüpheli odağın tam yeri bulunabildiğinden çok sayıda parça almak yerine bu yöntemle daha az örnek alınması yeterli olabilmektedir.
Füzyon biyopsi uygulaması iki yöntemle yapılabilir. Bunlardan birisi perineal bölgede ciltten girilerek yapılan transperineal yöntemdir. Bu yöntem genel veya lokal anestezi ile yapılabilir.
Diğer yöntem ise rektumdan girilerek yapılan transrektal yöntemdir. Bu yöntem de lokal anesteziyle yapılabilmektedir.
Prostat Kanseri Evreleri
Gleason Skoru Nedir?
Gleason Skoru, kanser hücrelerinin çoğalma ve yayılım hızını belirten bir terimdir. İngilizce kökü "grade" yani "derece" kelimesinden türetilmiştir. Gleason skorlaması, kanserin agresifliğini saptamak için kullanılır.Gleason skoru, kanser evresiyle aynı şey değildir. Prostat kanserinde evreleme; kanserin mevcut durumunun tespiti için yapılırken, Gleason skoru ise kanserin yayılma hızının belirlenmesinde kullanılır. Yani prostat kanserinde Gleason skoru, hastalığın seyir hızıyla ilgili bilgi sağlar.
Prostat kanserinde evreleme TNM tekniğiyle yapılır. T harfi tümörü temsil ederken, N harfi lenf nodülünü ve M harfi uzak metastazları temsil eder. Kanserin mevcut durumu, ne kadar alanı etkilediği TNM evrelemesiyle belirlenirken, kanserin bu aşamadan sonra ne hızla ilerleyeceği Gleason skoruyla saptanır.
Yüksek Gleason skoru, kanser hücrelerinin yayılma hızının yüksek olduğunu ifade eder. Düşük Gleason skoru ise benzer şekilde düşük kanser yayılma hızını gösterir. Puanlar 1'den 5'e kadar agresifliği temsil eder. Genellikle 1 ve 2 Gleason derecesi görülmez, 3, 4, 5 dereceleri kullanılır. Gleason skoru, biyopsi materyalinde en sık saptanan iki hücresel paternin agresifliklerinin toplanmasıyla elde edilir. Toplam değeri olarak Gleason skoru 6 ise görece düşük seyir ve yayılma hızını, Gleason skoru 10 ise yüksek seyir ve yayılma hızını gösterir. Yüksek Gleason skorları yüksek riskli tümörler olarak adlandırılır.
Gleason skoruna benzer şekilde ISUP sınıflandırması da kullanılabilir. Bu sınıflandırmada, 1'den 5'e kadar puanlama yapılır. 5, en hızlı seyreden agresif prostat kanserleri için kullanılırken, 1 en düşük hızda seyreden prostat kanserleri için kullanılır.
Gleason skorunun düşüklüğü ya da yüksekliği, hekim tarafından prostat kanserinin evresiyle birlikte değerlendirilmelidir.
PSA Nedir?
PSA yani Prostata Özgü Antijen, prostat bezinde üretilen bir proteinin kan testleri ile belirlenebilen değerini ifade eder. PSA değerinin yüksekliği; prostata dair hastalıkların ve kanser riskinin göstergesidir. Prostatın iyi huylu tümörlerinde ve prostat büyümesi durumunda da PSA değeri yükselebilir. Öte yandan PSA değeri normal aralıklarda seyrederken, prostat kanseri gelişmesi de olasıdır. PSA değeri tek başına prostat kanseri teşhisinde yeterli değildir.Prostat Kanseri Evreleri
Her kanser türünde olduğu gibi, prostat kanserinde de teşhis sonrası tedavinin belirlenebilmesi için kanser evrelemesi yapılır. Prostat kanserinin evrelemesi TNM tekniğiyle yapılmaktadır.
TNM tekniği, İngilizce bir kısaltmadan meydana gelmektedir. Açılımı şu şekildedir:
T- Tümör (Tumor): tümörün boyutu ve yerini ifade eder.N- Lenf Nodülü (Node): kanserli hücrelerin lenf düğümlerine ve lenf sistemine yayılımını ifade eder.M- Uzak Metastaz (Metastasis): kanserli hücrelerin uzak organ ve dokulara yayılımını ifade eder.Prostat kanserinin evresini saptamak, uygun tedavinin uygulanması ve hastalığın seyrini takip etmek açısından çok önemlidir.Evre 1Prostat kanserinin erken evresi sayılan bu evrede, tümör prostatla sınırlıdır. Tümör, rektal muayene ile hissedilemeyecek derecede küçük olabileceği gibi prostat bezinin sadece sağ veya sol tarafında olabilecek şekilde muayenede veya görüntülemede sağtanmış olabilir. Lenf nodlarına sıçrama veya vücudun diğer bölgelerine yayılımı yoktur. Prostat kanserinin birinci evresinde PSA değeri yüksekliği bulunmayabilir.
Evre 2Prostat kanserinin 2. evrede tümör prostatın içine doğru ilerlemiştir ancak hala prostatla sınırlıdır. Bu evrede tümör rektal muayene ya da görüntüleme yöntemleri (MR) tespit edilebilir. Lenf nodlarına sıçrama veya vücudun diğer bölgelerine yayılımı yoktur. Prostat kanserinin 2. Evresi gleason skorunun yüksekliğine göre 3 alt başlıkta değerlendirilir.
Evre 2a: PSA değeri 10-19 aralığındadır. Gleason skoru 6’dan yüksek değildiEvre 2b: PSA değeri 20 değildir. Gleason skoru 3+4=7’dir.Evre 2c: PSA değeri 20 değildir. Gleason skoru 4+3=7 veya 8’dir.Evre 3Üçüncü evrede tümör prostat kapsülünün ötesine ve seminal vezikül (sperm kesesi) gibi dokulara yayılmış olabilir. Lenf nodlarına sıçrama veya vücudun diğer bölgelerine yayılımı yoktur. Ancak PSA değerinde ve Gleason skorunda yükselme başlamıştır. Bu da tümörlü dokuların yayılım hızının arttığını gösterir. Prostat kanserinin 3. Evresi kendi içinde 3 kısımda değerlendirilir.
Evre 3a: Kanser prostatla sınırlıdır. PSA değeri 20’nin üstündedir. Gleason skoru 8 ve daha yüksektir.Evre 3b: Kanser prostat bezinin dışındaki dokulara yayılmaya başlamıştır ancak lenf nodu tutulumu yoktur. PSA değerinin yüksekliğine bakılmaz. Gleason skoru 8 ve daha üstündedir.Evre 3c: Kanser prostat bezinin dışındaki dokulara yayılmıştır ancak lenf nodu tutulumu yoktur. Gleason skoru 9 veya 10’dur.Evre 4Prostat kanserinin 4. Evresinde, tümör prostatın dışındaki dokulara, lenf düğümlerine ve uzak organlara yayılım göstermiş olabilir. Prostat kanserinin ilerlemiş son evresi olan dördüncü evre kendi arasında iki kategoriye ayrılır.
Evre 4a: Kanser yakın lenf düğümlerini tutmuştur. Yakın dokularda yayılımı bulunabilir.Evre 4b: Kanser uzak organlara metastaz yapmıştır. Uzak organ ve dokular, diğer lenf düğümleri ve kemiklerde kanser tutulumu bulunabilir.Prostat Kanseri Tedavisi
Prostat kanseri tespit edildikten sonra tedavi, hastalığa bağlı faktörler (evresi, yaygınlığı) ve hastaya bağlı faktörler (genel durumu, yaşı, ek hastalıkları) göz önünde bulundurularak planlanır.
Prostat Kanserinin Ameliyat Dışında Tedavi Şekli Mümkün Müdür?
Prostat kanserinin tedavisi; ameliyat, radyoterapi, hormonoterapi şeklinde düzenlenebilmektedir. Hastanın içinde bulunduğu şartlar ve genel durumu göz önüne alınarak tedavi şekli belirlenir.
Prostat Kanseri Vakalarında Günümüzde Sık Kullanılan Tedavi Şekli Hangisidir?
Günümüzde prostat kanseri tarama testlerinin kullanımının artmasıyla erken evrede saptanabilmektedir. Çevreye yayılmamış erken evredeki (lokal) prostat kanserinde en sık kullanılan tedavi cerrahi tedavidir. Gereği halinde hormon terapisi veya radyoterapi ile kombine edilebilmektedir.
Aktif İzlemProstat kanseri Evre 1’de yavaş ilerler, bazen hiç belirti vermez ya da sağlık şikayetlerine yol açmaz. Doktorunuz bu evrede PSA değeri, rektal muayene ve ultrason gibi yöntemlerle kanserin ilerlemesini takip eder. Aynı zamanda tümörün yayılma riski (skorlama) değerlendirilir.
Aktif izlemde amaç yavaş ilerleyen ve düşük riskli olduğu tespit edilmiş hastaların gerektiğinde tedavi şansını kaybetmeyecek şekilde yakından takip edilmesidir. Bu sayede bir grup hastanın gereksiz tedavi alması önlenmiş olur.
NanoknifeNanoknife (nanonayf okunur) yöntemi, klinik olarak anlamsız tümör denilen küçük hacimli düşük riskli prostat kanserlerinin tedavisinde kullanılmaya başlanmıştır. Bazı karaciğer ve pankreas tümörlerinde de uygulanan bu yöntem, prostat kanserinin tedavisinde de güvenle uygulanmaktadır.
Nanoknife yönteminde 3-4 tane özel elektrot, ultrason yardımı ile prostatta bulunan tümörün çevresine yerleştirilir ve bu elektrotlara sırayla çok yüksek dozda (3000 volt-50 amper gibi); ancak kısa süreli elektrik akımı verilir. Bu bölgede elektromanyetik bir alan oluşur ve hücre duvarı geçirgenliği kalıcı olarak artar. Bu şekilde tümör hücreleri canlılıklarını kaybederler.
Bu yöntem dokularda ısı değişikliğine sebep olmadığı için sinirlere ve üretraya (mesaneden dışarıya açılan ve prostatın da içinden geçen tüp şeklindeki yapı) yakın tümörlere de uygulanabilir.
Bu yöntemle tedavi edilecek hastalar iyi seçilmelidir. Normalde aktif izlem yapılabilecek hasta grubuna kullanılabilecek bir tedavi yöntemidir.
Yapılan işlem sonrası prostatta sadece kanserli hücreler tahrip edildiğinden ilerleyen zamanda prostat dokusunun başka bir bölgesinden kanser gelişme riski vardır. şayet böyle bir durum gelişirse hastaya küratif (cerrahi, radyoterapi) tedavi planlanır. Yani bu yöntem, küratif tedavi gerekebilecek hastalarda bu tedavinin olabildiğince ertelenmesini sağlamaktadır. Bu şekilde küratif tedavilerden doğabilecek bazı yan etkilerin de ertelenmesi amaçlanır.
Prostat Kanserinde Cerrahi Tedavi - Radikal Prostatektomi
Yayılım göstermeyen prostat kanserinin tedavisinde, cerrahi olarak prostatın çıkarılmasıdır. Bu cerrahiye radikal prostatektomi ameliyatı denir. Radikal prostatektomi operasyonu geçiren düşük dereceli tümöre sahip hastaların 10 yıllık hastalığa özgü sağ kalım oranları %90’ın üzerindedir.
Prostat çıkarılırken idrar tutmaya yarayan yapılara zarar verilmemesi ve sinirlerin korunması önemlidir.
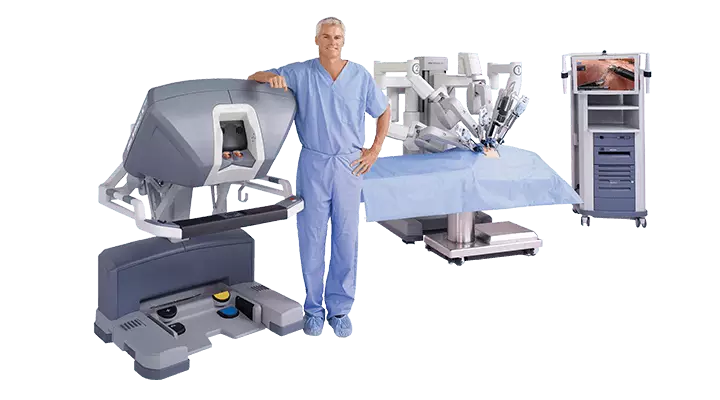
Robotik Cerrahi Ne Demektir?Robotik cerrahi, laparoskopik (kapalı) ameliyatların “da Vinci” isimli robot yardımıyla 3 boyutlu görüntü altında yapılmasıdır. Laparoskopik yapılabilen birçok ameliyat (ürolojik, genel cerrahi, kadın hastalıkları vb.) bu yöntemle yapılabilmektedir.
Robotik Cerrahide Cerrahın Fonksiyonu Nedir?Robotik cerrahi denilince ameliyatın robot tarafından yapıldığı şeklinde yanlış bir kanı vardır. Oysa ameliyatı gerçekleştiren kişi robot değil cerrahın kendisidir.
Robotik Cerrahi ile Prostat Kanseri Ameliyatının Komplikasyonları Nelerdir?Prostat dokusunun bulunduğu anatomik yerleşim, ereksiyonu ve idrar tutmayı sağlayan yapılara çok yakındır. Bu sebeple prostat cerrahisinin en önemli komplikasyonları ameliyat sonrası ereksiyon kaybı ve idrar tutamama (inkontinans)’dır.
Robotik cerrahi ile prostat ameliyatındaki asıl amaç prostatın geride kanserli doku bırakmayacak şekilde çıkarılması, cinsel fonksiyonların devamını sağlayan sinirlerin korunması ve prostat çıkarılırken idrar tutmayı sağlayan yapılara zarar verilmemesi olarak sıralanabilir.
Mesane ile prostat arasında bulunan bir anatomik planın ortaya koyulması ile robotik prostat ameliyatlarında “Mesane Koruyucu Teknik” tanımlanmıştır. Bu teknikle yapılan ameliyat sonrası hastalarda idrar tutamama oranları çok azalmıştır.
Robotik Cerrahinin Açık Ameliyattan Farkı Nedir?Geleneksel açık cerrahi yöntemde hastanın göbek altından yaklaşık 15 cm’lik bir kesi yapılır. Açık ameliyatın hem hasta hem de cerrahi ekip için birçok zorluğu bulunmaktadır.
Operasyondan sonra geç iyileşme süresi, uzun süre hastanede kalış, yara enfeksiyonu riski ve büyük bir yara izi bu cerrahinin hasta adına zorlukları olarak sayılabilir.
Cerrahi alanın darlığı sebebiyle el hareketlerinin yetersiz kalması ve iyi bir görüş alanının sağlanamaması sebebiyle ameliyat sürelerinin uzun olması ve komplikasyon oranlarının artması ise cerrahi ekip adına sayılabilecek zorluklardır.
Robotik cerrahi, Da Vinci adı verilen bir robotun hasta üzerine uygun şekilde yerleştirilmesi ve bu robotun kollarının, konsol cerrahı tarafından, konsol adı verilen kontrol ünitesinden yönlendirilmesi ile gerçekleştirilen bir ameliyat şeklidir. Genel prensipleri laparoskopik cerrahiye benzemektedir.
Robotik cerrahide kullanılan ameliyat kollarının ince yapısı, hareket kabiliyeti, titreşim engelleyici çalışma prensibi ve robotik sistemin gelişmiş görüntü sistemleri sayesinde prostat ameliyatı sırasında prostata yakın komşuluktaki yapılar daha rahat korunabilir olmuştur. Böylece ameliyat sırasında komplikasyon ihtimali aza inmekte, kan kaybı azalmakta ve ameliyat süresi kısalmaktadır.
Ameliyat sonrası ise ağrıda azalma, iyileşme süresinin kısalması, ilerleyen dönemde cinsel fonksiyonların kaybı ve sürekli idrar kaçırma gibi sosyal yaşantıyı büyük ölçüde etkileyen sağlık problemlerinin azalması gözlemlenmektedir.
Ameliyat hangi teknikle yapılırsa yapılsın, robotik cerrahi ile prostat kanseri ameliyatı sırasında da dikkat gerektiren aşamalar vardır.
Burada asıl amaç prostatın geride kanserli doku bırakmayacak şekilde çıkarılması, cinsel fonksiyonların devamını sağlayan sinirlerin korunması ve prostat çıkarılırken idrar tutmayı sağlayan yapılara zarar verilmemesi olarak sıralanabilir.
RadyoterapiRadyoterapi (ışın tedavisi) kanser hastalığının radyasyon kullanılarak tedavi edilmesidir. Radyoterapinin amacı normal dokuya mümkün olduğunca az zarar vererek, kanserli hücreleri öldürmek veya bölünüp çoğalmalarını engellemektir.
Radyoterapi, cerrahi yöntemlere benzer şekilde lokal bir tedavi yöntemidir; etkisini de, yan etkisini de uygulandığı yerde göstermektedir. Lokalize prostat kanserinde radyoterapi, küratif bir tedavi yöntemi olarak kullanılmakla beraber, prostat komşu organlarına (lokal ileri) ve uzak organlara yayılmış (metastatik) hastalarda da palyatif (ağrı gibi şikayetlerin giderilmesine yönelik) ya da tümör yükü azaltma amaçlı tedavi olarak kullanılabilir.
Radyoterapinin Yan Etkileri Nelerdir?Radyoterapinin yan etkileri genellikle ilk günlerde değil, ilerleyen günlerde, doz arttıkça başlar. Her zaman meydana gelmeyeceği gibi kişilere göre de değişiklik gösterebilir.
Genel yan etkilerden bazıları ciltte irritasyon (rahatsızlık) ve yorgunluk hissidir. Prostat kanserinde kullanılan radyasyon tedavisi, erektil disfonksiyona (sertleşme bozukluğu) ve inkontinansa (idrar tutamama) sebep olabilir. Bunun dışında da sık idrara çıkma hissi ve idrarda kanama görülebilecek bazı durumlardır.
Kemo-Hormono TerapiProstat kanserinin ilerlemiş safhalarında hastalık prostata sınırlı kalmayarak komşu dokulara ve uzak organlara yayılmış olarak tespit edilebilir. Hastalığın bu safhasında cerrahi yöntemler yetersiz kalacağından ilaç tedavileri tercih edilir.
Prostat dokusu erkeklik hormonu testosterona duyarlı bir organ olduğundan, hastalığın bu safhasında testosteron etkisini engelleyen ilaçlar (anti-androjen) kullanılır. Bu tedaviye hormonoterapi (hormon terapisi) denir.
Bu tedaviye yanıtsız olan veya direnç kazanan hastalara ise kemoterapi planlanır. Bu şekilde ileri evre prostat kanseri olan hastaların da yaşam sürelerinin uzatılabildiği bilimsel çalışmalarla ortaya koyulmuştur.