Breast diseases, especially breast cancer, are among health problems with constantly increasing incidence in general population. Acıbadem Healthcare group provides patients with most up-to-date diagnosis and treatment services for various breast diseases and breast cancer by physicians through is medical technology infrastructure and service approach focused on patient safety.
In addition to treatment of breast diseases and breast cancer, breast-sparing surgical procedures are carried out to protect appearance of breasts along with psychological support to have many patients cope with this period of life more easily at Acıbadem.
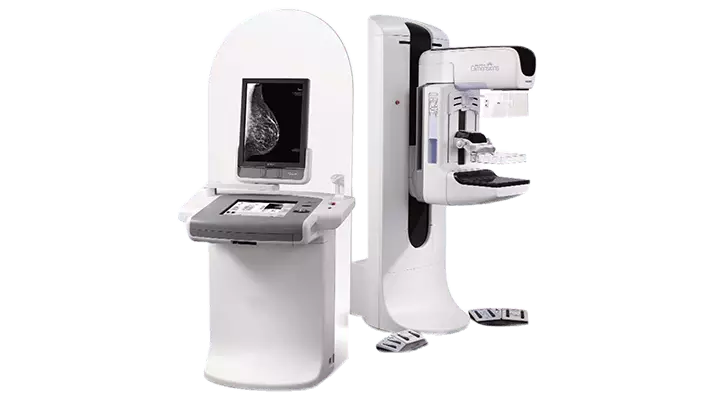
Acıbadem Healthcare Group have already installed many devices needed in field of breast health to detect and treat tumors, such as 3D Tomosynthesis Digital Mammography and Single Dose Radiotherapy that is used in surgery in order to render all services patients may need in treatment.
Versatile Approach
Diagnosis and treatment of breast cancer requires multidisciplinary approach, where physicians specialized in various fields exchange opinions and decisions are made jointly. This approach ensures that relevant physicians start treatments after a consensus is reached on diagnosis and treatment of each patient.
A team of general surgery, plastic surgery, radiology, pathology, medical genetic, medical oncology and radiation oncology physicians use technological infrastructure to provide patients with diagnosis and treatment services at these units. In addition, treatment process is backed up with dietary consultation, psychological counseling and physical medicine and rehabilitation programs.
Diagnosis and Treatment Services
Among the services available for diagnosis of breast cancer at our hospitals are clinical examination of breast, 3D tomosynthesis digital mammography, 4D ultrasound and biopsy. Breast cancer screening programs are developed by educating patients on self-examination of breast within scope of preventive healthcare services.
Moreover, women who are at high risk of breast cancer are followed up regularly along with personalized counseling. Here, it is aimed to ensure early diagnosis for women who are at risk in order to minimize future onset of breast cancer in such women.
Breast-sparing and Oncoplastic Surgery
Total removal of breast due to cancerous tissue is an undesired condition for many women. Loss of breast may adversely affect body image in psychological terms. Therefore, breast-sparing surgery is preferred as much as possible in contemporary management approaches.
General surgeons of Acıbadem use oncoplastic surgery and innovative reconstructive techniques especially for patients with breast cancer. When required, plastic and reconstructive surgeons are involved in treatment to restore natural look of breast through surgical touches.
Treatment Options by Condition of Disease
Surgical procedures are first preferred for treatment of breast cancer diagnosed at early stages. Generally, surgical management is immediately followed by systemic treatments, such as chemotherapy and/or hormone therapy. Radiotherapy is frequently preferred in treatment of cancer to kill cancer cells and destroy tumors.
Treatment Methods of Breast Cancer
Various methods are used to manage breast cancer. Although treatment modalities vary depending on course of disease, these are surgery, medication therapy (chemotherapy), hormonotherapy (treatments with hormone drugs), radiotherapy and biologic treatments to list a few. The first-line treatment is dictated by clinical stage of the disease.
Cerrahiye Hangi Durumlarda Başvuruluyor?
Acıbadem Kayseri Hospital Genel Cerrahi Uzmanı Prof. Dr. Can Küçük; "Meme Kanseri" üzerine soruları cevaplıyor.Surgery is the first option for breast cancers diagnosed at early stages. Considering surgical approach, either breast tumor is removed, but a safety zone of healthy tissue is left or entire breast is excised. Moreover, some lymph nodes are dissected to understand whether tumor has spread to armpits or not..
First, stage of disease is determined following the surgery to decide extra treatments (radiotherapy, hormone therapy, chemotherapy) that are required.
Today, very successful outcomes are obtained in many patients thanks to advancements in surgery techniques and adjunctive therapies.
Is Entire Breast Removed?
In the past, it was thought that there was no option other than removal of entire breast (mastectomy) and complete dissection of axillary lymph nodes. However, it is, nowadays, preferred only for a couple of patients, if the condition is diagnosed at early stages.
For one out of every two patients, it is possible to spare the breast by removing the tumor followed by breast radiotherapy. Breast-sparing treatment does not significantly differ from total removal of breast in selected patients.
Breast Surgery
Considering treatment of breast cancer, surgery is the first option for breast cancers diagnosed at early stages. Considering surgical approach, either breast tumor is removed, but a safety zone of healthy tissue is left or entire breast is excised. Moreover, some lymph nodes are dissected to understand whether tumor has spread to armpits or not. First, stage of disease is determined following the breast surgery to decide extra treatments (radiotherapy, hormone therapy, chemotherapy) that are required.
Today, very successful outcomes are obtained in treatment of breast cancer for many patients thanks to advancements in surgery techniques and adjunctive therapies.
Memede Bir Kitle Tespit Edildiğinde Mutlaka Alınmalı Mıdır?
Acıbadem Bursa Hospital, Genel Cerrahi Uzmanı Prof. Dr. Abdullah Zorluoğlu, Kanser üzerine soruları yanıtlıyor.Breast-sparing Surgery
Patients with breast cancer die due to systemic recurrence, also called metastasis, rather than local relapses in breast. In this sense, surgery techniques that focus on removal of tumor through a breast-sparing approach are preferred over total removal of breast in selected cases with single tumor. In breast sparing surgery, tumor tissue is removed along with approximately 1- to 2-cm healthy breast tissue surrounding the tumor (large excision, tumorectomy, and lumpectomy).
Other techniques that enable larger removal of the diseased part in breast are called “quadrantectomy” or “partial mastectomy”.
Non-palpable lesions which are considered malignant and marked with wire under mammography or ultrasound scans are removed under guidance of wire or ROLL (Radionuclide-Guided Occult Lesion Localization) technique; and next, X-ray is scanned to confirm removal of the lesion.
Meme Kanserinin Cerrahi Tedavisinde Memenin Tümünün Alınması Ne Zaman Gerekli Oluyor?
Acıbadem Maslak ve Bakırköy Hastaneleri Genel Cerrahi Uzmanı Prof. Dr. Cihan Uras, meme kanserinin cerrahi tedavisinde memenin tümünün alınmasıyla ilgili açıklama yapıyor..Who are good candidates?
In treatment of breast cancer, breast-sparing surgery should generally be performed in selected patients: the disease is at early stage (stage I-II) and tumor/breast ratio is appropriate; there is single-focus small tumor; and postoperative radiotherapy is planned for the patient. Annual rate of relapse in same breast is 0.5-1 percent following breast-sparing surgery, but it may vary according to characteristics of tumor.
What should be taken into account?
In management of breast cancer, it is necessary to ensure that patients are informed before surgery, radiotherapy may be required and the patient will present for follow-up visits. It is essential to follow up patients carefully for a long time. If patient will receive chemotherapy after surgery, chemotherapy is followed by radiotherapy.
Treatment is planned through multidisciplinary approach for breast cancer. Physicians of general surgery, radiology, pathology, medical oncology and radiation oncology clinics work in cooperation through a multidisciplinary approach to plan treatment of breast cancer. Considering treatment of breast cancer, patients are mostly examined first by a general surgeon. Another important aspect of treatment is to have patients evaluated by psychologists and psychiatrists before and after treatment..
Mastectomy
Although mastectomy (surgical removal of entire breast) had been widely used in the past, it is, nowadays, preferred for a large tumor and/or multi-focus tumors that involve breast diffusely, as breast-sparing surgery is not appropriate for latter cases.
Such surgeries may be performed in the form of “nipple sparing mastectomy” to preserve skin of breast in early stage tumors or if the tumor is located distant to the nipple.
Meme Kanserinin Cerrahi Tedavisinde Memenin Alınması Her Zaman Gerekli Mi?
Acıbadem Maslak ve Bakırköy Hastaneleri Genel Cerrahi Uzmanı Prof. Dr. Cihan Uras, Meme kanserinin cerrahi tedavisinde memenin alınması konusunda açıklama yapıyor.Surgical Procedures for Armpits
a- What is Sentinel Lymph Node Biopsy (SLNB)?
Breast cancer most commonly spreads to lymph nodes of axillary fossa (armpit). In the past, removal of all axillary lymph nodes (axillary dissection) was preferred to stage the disease, determine involvement of axillary lymph nodes and ensure local control. However, side effects of this procedure, including but not limited to swollen arm (lymphedema), limited range-of-motion and deformity in shoulders, weakness of muscles in arms and numbness have steered research to novel modalities.
Recently, “Sentinel Lymph Node Biopsy Technique” was developed that implies removal of lymph nodes, which are most likely to be invaded by tumor cells.
How is Sentinel Lymph Node Biopsy Technique Performed?
In this technique, a radioactive substance is preoperatively injected into the location of tumor in breast. Following lymphoscintigraphy one day before the surgery or on the morning of surgery if it is scheduled to be performed in the afternoon, the lymph node(s) with high radioactive substance (tracer) activity are detected by a radioactive substance detector or counter, called gamma probe, and they are surgically removed and sent to pathology laboratory for relevant tests and examinations.
A blue dye can also be injected to the breast with tumor in the surgery. In this case, the blue stained lymph duct is identified and tracked to remove blue stained lymph node(s) that is/are called sentinel lymph node and the specimen is again sent to pathologist while the surgery continues. All axillary lymph nodes are removed, if sentinel lymph node is involved.
In case of negative biopsy result, the tissue is left untouched and lymph nodes are not dissected that are considered clean. Thus, certain side effects such as lymphedema, restricted range-of-motion in shoulder or numbed arm are very rare in patients, if only sentinel lymph node biopsy is performed.
However, these sentinel lymph nodes are subjected to special treatments and advanced staining techniques are performed for negative specimens. Consequently, a second surgery is considered and complementary axillary dissection is performed or in other words, all lymph nodes are dissected, if minimal involvement is detected in lymph nodes.
What Are Indications of Sentinel Lymph Node Biopsy Technique?
Axillary lymph nodes are involved less than 50 percent in T1/T2 tumors that are smaller than 5 cm. Therefore, sentinel lymph node biopsy should be performed for all T1/T2 cases, especially if clinical examination and/or ultrasound scan does not point to suspicion of axillary lymph node involvement.
Since studies on patients without any tumor in axillary lymph nodes could not reveal out a difference regarding axillary local recurrence in long-term outcomes of patients in groups of sentinel lymph node biopsy or axillary dissection, it is possible to mention that sentinel lymph node biopsy alone is the standard approach for clinically axilla-negative patients.
b- Removal of Axillary Lymph Nodes (axillary curettage, axillary dissection)
It refers to dissecting most of the axillary lymph nodes in case of axillary lymph node involvement. In such cases, some patients may experience certain complaints, such as swelling, numbness or tingling in arms secondary to dissection of lymph nodes.
Breast Reconstruction
Breast reconstruction is performed to restore natural form of the breast that is defective due to breast cancer. This point of view suggests that breast reconstruction should be deemed a reconstructive surgery, which implies restoration of a limb lost due to a disease, rather than a cosmetic surgery.
Plastic and reconstructive surgeons are also in the treatment team of breast cancer. Aforementioned physicians perform surgeries which restore breast of patients to the natural form, if required.
Surgeons can construct breasts which look very natural thanks to recent advancements in medicine.
Reconstruction of Breast Tissue
Selection of surgical technique and appropriate time of repair surgery are dictated by certain criteria. A series of factor play a role in the decision process, including but not limited to overall health of patient, age, body characteristics, features of mastectomy, whether radiotherapy is required or not, condition of other breast, preference of patient and experience and skills of the plastic surgeon.
Memenin Tümünün Alındığı Durumlarda Aynı Seansta Meme Yapabilmek Mümkün Mü?
Acıbadem Maslak ve Bakırköy Hastaneleri Genel Cerrahi Uzmanı Prof. Dr. Cihan Uras, memenin tümünün alındığı durumlarda aynı seansta meme yapımıyla ilgili bilgi veriyor.Breast implants
There are two main types of breast implants: Ones filled with gel and ones with saline. Exterior surface is made of silicone membrane in both types of implants. Breast can be reconstructed directly by placing implants (in simultaneous reconstructions) or a “tissue expander” is placed to expand soft tissues of chest wall and next, it is removed to make a room for placement of breast implant. This method is preferred especially for late-stage reconstructions.
Reconstruction surgery with breast implant is technically a simple and short-lasting method. However, a foreign body is surgically placed into the body and these reconstructions may cause certain complications, such as infection, silicone leak or deflation of implant. Another adverse outcome of this technique is failure to create a natural look due to development of solid tissue around the silicone implant.
Breast Reconstruction with the Patient’s Own Tissue (Autogenous Tissue):
Breast reconstructions with autogeneous tissue are more complex surgeries that require surgical experience. Autogeneous tissue is usually obtained from abdomen, back, hip and leg. These are:
Abdominal skin and subcutaneous adipose tissue in lower part of abdomen and one of the anterior abdominal wall muscles (transverse abdominis muscle (TRAM)) are transferred to breast region in the form of pedicled or free flap (free tissue transfer—microsurgery) and breast reconstruction is performed. Tummy tuck surgery is also performed in this surgery.
The muscle at lateral part of the back (latissimus dorsi muscle) and the skin that covers this muscle are transferred in the form of pedicled or free flap (free tissue transfer – microsurgery) and used for breast reconstruction. In this technique, the incision scar is usually concealed by bra.
Breast can also be reconstructed by transferring skin and subcutaneous adipose tissue of hip and leg free tissue transfer or microsurgery technique – to breast region.
Microsurgery
In breast reconstruction with free tissue transfer technique, skin and subcutaneous fat tissue, also including feeder arteries, are elevated from abdomen, back or hip region and their viability is ensured by anastomosing feeder arteries of the graft to the arteries of the recipient site. Plastic surgeon should be experienced in microsurgery to perform this surgery. Because thin vessels can be sutured only under microscope.
Autogeneous tissues are pretty similar to breast tissue with regard to content. Based on these characteristics, physical behavior of a breast that is reconstructed using autogeneous tissues will resemble the natural breast better and the sensation is restored better and quicker than breast implant surgeries. Satisfaction with outcome will increase when incision scars fade and the tissues used for the reconstruction soften in the postoperative period.
Autogeneous tissues are identical to the normal breast in terms of the respond to weight loss and gain. As a result, symmetry of both breasts can be maintained in case of sagging secondary to excessive weight gain or loss as well as aging after reconstructive surgery. Moreover, breasts reconstructed with autogeneous tissues do not create a contraindication to radiotherapy or chemotherapy.
Reconstruction of Nipple and Areola
Several surgeries may sometimes be required to achieve a breast with natural look. The most complicated one is the first surgery, in which breast tissue is constructed. Second surgery is performed to reconstruct nipple and areola (the darker area surrounding the nipple) under local anesthesia and it is easier than the first one. Nipple is constructed using local tissues. Tattoos can be used to replace areola or cutaneous graft can be obtained from nipple of other breast or groin.
Memenin Tümünün Çıkarılması Gerekli Olduğu Durumlarda Meme Başı Bölgesinin Alınması Gerekiyor Mu?
Acıbadem Maslak ve Bakırköy Hastaneleri Genel Cerrahi Uzmanı Prof. Dr. Cihan Uras, memenin tümünün çıkarılması gerekli olduğu durumlarda meme başı bölgesinin alınmasıyla ilgili açıklama yapıyor.Achieving Symmetry of Breasts
Symmetry of the repaired breast with other breast is not expected in case of unilateral breast reconstruction. This also applies even if other breast is large or sagging. In this case, certain surgeries can be carried out for other breast to achieve symmetry of breasts. These include breast reduction, breast lift (mastopexy) or breast augmentation.
Postoperative period of breast surgery
Postoperative pain is largely managed by medicines. Hospital stay is dependent on complexity of surgery; it may be necessary to stay at hospital 1 to 2 days, if reconstruction is not performed, or otherwise, hospital stay is 2 to 5 days. Patients are discharged 1 day after operation, if breast-sparing surgery is performed, or patients are discharged in 1 to 2 days. Drains are generally placed to prevent collection of fluid and they are usually removed several days to 1-2 weeks after the surgery depending on the surgery technique.
Getting Back to Daily Activities
Although return to daily activities after the surgery varies according to surgery technique in treatment of breast cancer, it usually takes several days to 4 weeks. For autologous reconstruction patients, hospital stay may be longer relative to breast reconstruction with implants.
Patients can take a bath as usual 2 days after the surgery, even if drain is not removed, provided no water should leak into drains. Wound dressing on drains should be changed after each shower. Although contact of surgical wounds with water does not cause any problem as of 2 days after the surgery, it is necessary to avoid severe irritation of the wound.
No food restriction or a special diet is required, starting several hours after the surgery.
Normal senses cannot be restored with reconstruction surgery, but it may recover slightly over time. Scars mostly fade over time. However, scars never disappear, even if fading takes 1 to 2 years. Patients pay less attention to scar formation as long as the quality of repair is high.
Chemotherapy for Breast Cancer
Patients receive chemotherapy before or after surgery for treatment of breast cancer and moreover, these two modalities are followed by hormonotherapy. Age of patient, size of tumor and biological/pathological characteristics of tumor play an important role in selection and duration of treatment.
Tüm Meme Kanseri Hastaları Kemoterapi Almalı Mıdır?
Acıbadem Bursa Hospital, Genel Cerrahi Uzmanı Prof. Dr. Abdullah Zorluoğlu, Kanser üzerine soruları yanıtlıyor.Chemotherapy is mostly started after surgery in breast cancer. Excluding certain special conditions, chemotherapy is usually the first-line treatment for patients with locally advanced breast cancer that is inoperable or advanced stage breast cancer that has already metastasized to other organs.
Hormone Therapy in Breast Cancer
Considering treatment of breast cancer, patients with estrogen- and/or progesterone-positive tumors, who are undergone surgery and received chemotherapy, are given hormone drugs (hormone therapy) that are structurally similar to these hormones, but suppress them.
Tamoxifen is among medicines with proven value in hormone therapy that is another arm of the system therapy; it is used in premenopausal patients for 5 years.
Targeted Biological Therapies
Both chemotherapy and hormone therapy affect the whole body and have systemic effects. Targeted treatments, on the other hand, directly focus on the cancerous tissue and aim to destroy the tumor alone and minimize the systemic effects by using drugs that target markers of the tumor.
Who are good candidates?
There are various methods for targeted biological therapies. The primary one is an antibody that is globally acknowledged and administered to suppress c-erbB2 (HER-2 neu) protein in patients with breast cancer characterized by overexpression of this protein. C-erbB2 protein is present in approximately 1/4 of breast cancer patients.
How long does it last?
It is intravenously administered indefinitely for patients with metastatic advanced stage disease and at 3-week or one-week intervals for 1 year in postoperative period for patients with early-stage disease.
What are side effects?
The most critical side effect of this treatment is cardiac dysfunctions.
If inflammatory breast cancer is present,
Clinical prognosis of locally advanced stage III inflammatory breast cancers can be poor. This group of patients is primarily started on chemotherapy due to very high risk of systemic metastasis and mastectomy and axillary dissection are required, if sufficient response is achieved. Postoperative chest wall radiotherapy is also very crucial for these patients. Moreover, targeted treatments and various hormone therapies can be started depending on characteristics of tumor.
Wrong
Radiation therapy burns and harms the breast skin.
Correct
In treatment of breast cancer, radiotherapy may lead to a temporary redness in skin which is similar to sunburn. Redness fades over time, after the treatment is completed.
Radiotherapy
Radiotherapy is a treatment modality that is used in approximately ¾ of all cancer patients. Given principles of multidisciplinary treatment, radiotherapy can be used alone for curative treatment or in combination with chemotherapy/systemic treatments before or after surgery. It is also used to help alleviation of complaints caused by the disease.
What is it?
Radiation Therapy, also called Radiotherapy, uses high-energy X-rays, electron bundles and radioactive isotopes to kill cancer cells and destroy tumors.
What is mechanism of action?
Radiation treatment damages the genetic materials of cells at the irradiated area and thus, division and proliferation of these cells are hindered. Radiation kills the cancer cells through ionization. Some cells die immediately, as they are directly affected by the radiation.
Chromosome and DNA of others are damaged and therefore, they lose reproductive capability and finally, they die. Although radiation treatment causes damage in healthy cells along with cancer cells, healthy tissues may recover and gain normal functions again.
Are There Different Radiotherapy Methods?
A successful treatment is characterized by ability to deliver the appropriate and efficient radiation dose to the tumor, while the dose exposed by surrounding healthy tissues is minimized. There are various methods to achieve these goals. The most common method is external radiotherapy which focuses radiation beams directly to the tumor.
Another method is brachytherapy. Intra-cavitary radiotherapy, which is one of brachytherapy methods, places an applicator which contains radiation seeds into an organ such as uterus, lung bronchus and esophagus. This method is generally used in combination with external radiation.
External radiotherapy is generally the most commonly preferred technique in breast cancer. However, brachytherapy methods can also be used in special circumstances depending on the physician’s preference.
How is treatment planned?
Patients who present with diagnosis or suspicion of cancer are primarily examined and undergo oncologic evaluation to determine a treatment protocol and next, radiotherapy is planned. All radiation treatments are programmed by expert physicians who are educated on this modality (radiation oncologists). Radiation oncologist cooperates with a team of medical physicist and radiotherapy technicians at the application phase of radiotherapy.
Meme Kanserinin Tedavisinde Ameliyat Sırasında Hangi Hastalara Radyoterapi Uygulanır?
Acıbadem Maslak ve Bakırköy Hastaneleri Genel Cerrahi Uzmanı Prof. Dr. Cihan Uras, meme kanserinin tedavisinde, ameliyat sırasında yapılan radyoterapi uygulamasıyla ilgili bilgi veriyor.When is it applied?
In treatment of breast cancer, radiotherapy generally plays a role after surgery and the technique is selected according to the surgical method. If the patient is undergone "breast-sparing surgery", radiotherapy is generally prescribed for almost all patients as a part of treatment in order to minimize risk of recurrence in breast tissue.
Now, single-dose radiotherapy in surgery is an acknowledged approach in patients who undergo breast-conserving surgery depending on technological means and age of patient as well as size and characteristics of tumor. If “mastectomy” is performed, chest wall radiotherapy can be considered, after diameter of tumor, other patient and tumor factors as well as involvement of lymph nodes are evaluated.
Radiotherapy can also be applied to lymph nodes depending on invasion of disease and location of tumor, if axillary lymph nodes are involved.
Preoperative radiotherapy may be rarely considered after chemotherapy for patients with regional or locally advanced cancer.
Radiotherapy plays an important palliative role to alleviate and eliminate complaints, if bone, brain and soft tissue metastases are detected in patients with advanced stage cancer.
How Long Does Treatment Last?
Radiotherapy is delivered once a day for 5 days a week, from Monday to Friday. Irradiation takes 3 to 4 minutes, although it may vary according to treatment plan and target zone. However, entire process is completed within 20-30 minutes, including patient’s placement on the treatment table, preparations and adjustment of treatment volume. Total duration of the treatment is decided by Radiation Oncologist. It is necessary for patients to continue the treatment regularly, excluding emergencies.
What are side effects?
Breast radiotherapy may sometimes cause redness and peeling in skin, tiredness, fatigue or nausea. These side effects gradually regress and disappear over time, after the radiotherapy is completed. Patients are allowed to take shower with warm water during the radiotherapy, but rubbing or use of bath puff with soap may irritate the target volume and make patient prone to skin reactions.
Hardness in breast tissue and pain are expected in the long-term secondary to surgery and radiotherapy, but these conditions mostly disappear within 6 months to 1 year, but they may persist longer in some cases. The dark discoloration of breast skin fades over time. In very rare cases, radiotherapy may lead to small red spots on breast skin due to rupture of capillaries. However, it is not an issue nowadays.
There are other side effects which may occur in the long term due to radiotherapy volumes or targets. These are generally caused by patient-specific factors. Patients are informed in detail by physicians regarding risk of side effects depending on the irradiated body part and what should be done in treatment.
Technologies Used For Radiotherapy
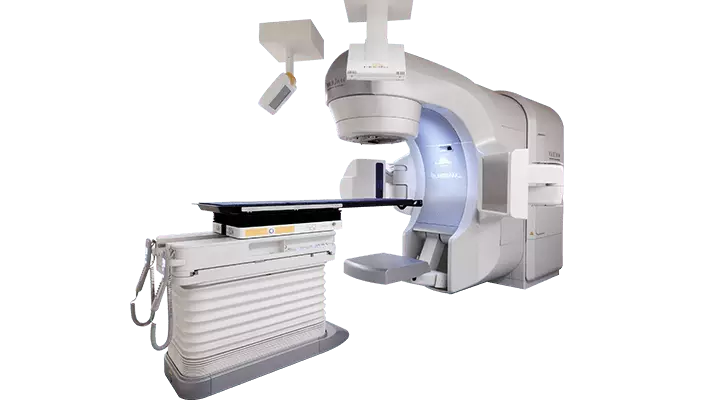
Linear accelerator: Linear accelerator device that generates high-energy X-ray is used for radiotherapy. Thanks to these devices, healthy tissues can be spared during radiation, while maximum dose can be directed to tumor tissue. Thanks to electronic portal imaging feature of linear accelerator which enables 3-dimensional conformal therapy, also called Intensity Modulation Radiation Therapy (IMRT), along with conventional treatment, target volumes of patients can be online imaged and checked.
In radiotherapy, treatment devices, called ‘linear accelerator’, have been used for approximately 50 years. Main mechanism of these devices is as follows. Electrons are accelerated and beams with different energy levels are directed to the tumor depending on needs of patients. Common features of these beams are high-energy, rapid penetration into body and ability to irradiate the whole body.
Recently, developments in computer technology are utilized in radiotherapy. Images acquired by computerized tomography scanner demonstrate the tumors in body. Radiation oncologists mark tumors and healthy tissues on cross-sectional images and next, radiation physicists plan treatment over these three-dimensional images.
In treatment, beams reach the tumor from various angles and a certain safety margin is left around the diseased region. Treatment aims to deliver maximal dose to the diseased body part for converting tumor into a harmless form. Another important goal is to spare the healthy tissue or organs from radiation. Radiation can be harmful for healthy tissues. If normal tissues are irradiated, side effects are more likely.
Recently, 3-dimensional conformal treatment and IMRT have been developed to conserve healthy tissues at maximum level and reduce adverse effects while irradiating the tumor at highest dose. With these methods, intensity of the radiation in target volume is adjusted and dose distribution is almost optimized. While tumor is irradiated at high doses, healthy tissues are conserved to the maximum extent. For example, these methods allow delivery of intended dose to the diseased breast, while lungs, heart, great arteries of heart and other breast are protected in breast radiotherapy..
IGRT Hinders Deviations During Treatment
It allows imaging the target volume before each radiotherapy session. Thus, treatment volume is located and position of the patient is corrected, if there is any deviation. Another advantage of this method is ability to acquire cross-sectional images during treatment. Thus, errors arising out of movement of organs at the periphery of treatment target and the tumor can be detected and corrected during treatment. Accordingly, tumor is irradiated, while damage to healthy tissues is minimized.
Single-dose radiotherapy delivered by linear accelerator implies use of radiotherapy at single dose during surgery.
Image Guided Radiotherapy (IGRT) with IMRT feature and portal kV imaging system, One Variant Trilogy, One Varian DHX RapidArc Linear Accelerator and Treatment Planning System
Varian Varisource HDR Brachytherapy that allows brachytherapy by placing a radioactive substance into body cavities or tissue.
In single-dose radiotherapy, radiotherapy is completed during a surgical procedure. After breast tumor is removed, the special applicator of the device is placed into the location of tumor. Following necessary measurements, high-dose radiation is delivered only to the target zone and therefore, healthy tissues are completely protected.
Conventional Radiotherapy
For patients with breast cancer, radiotherapy is applied using special devices that generate photon and electron, called “linear accelerator”, in specially shielded rooms at Radiation Oncology Departments. Almost all patients who are diagnosed with breast cancer and undergone “breast conserving surgery”, which implies removal of only tumor in breast, need postoperative radiotherapy.
Radiotherapy is preferably started after chemotherapy, if patient will be started on chemotherapy, or it is preferable started at least 3 weeks after surgery for patients who do not require extra systemic therapy or will receive only hormone therapy. For breast radiotherapy patients, computerized tomography is scanned at 2-5 mm intervals to plan the treatment.
Next, a plan is made to ensure delivery of necessary dose to the risky zones of breast, while healthy organs (heart, great arteries of heart, lungs, other breast that are metastasis-free) are conserved. After the plan is approved, patient is placed on radiotherapy that will last 5 to 7 weeks, depending on patient’s condition and discretion of radiation oncologist. For special cases, hypofractionated or short-term therapy is applied. This treatment lasts 2 weeks. Patient receives radiotherapy every day, excluding weekend.
SINGLE-DOSE Practice
As is the case with conventional radiotherapy, linear accelerator is used for single-dose radiotherapy. In this method, a portable linear accelerator that generates only electron energy is safely used in operating theater; this accelerator does not require as much radioactive protection equipment as conventional linear accelerators for healthcare personnel.
Surgery is carried out jointly by surgical team, radiation oncologist and medical physicist. It is advantageous for patients, as it is not necessary to wait for postoperative wound healing and patients do not need to visit hospital every day for planning and treatment. Thus, radiotherapy is completed during surgery.
After breast tumor is removed, the special applicator of the device is placed into the location of tumor. Following necessary measurements, high-dose radiation is delivered only to the target zone and therefore, healthy tissues are completely protected. Recently, Single-dose radiotherapy or irradiating the location of tumor rather than entire breast with different methods is globally acknowledged, but single-dose radiotherapy is not choice for all patients. Radiation oncologist of the patient, surgeon and pathologist should jointly decide whether this method is appropriate for the patient. Age of patient and pathological characteristics of tumor play important role in this decision.
EXTRA DOSE Therapy
Single-dose radiotherapy can be given in the form of extra dose therapy. Especially young patients (who meet certain criteria according to pathology report) may need local irradiation of tumor following whole breast radiotherapy after breast-conserving surgery. Treatment lasts approximately 6.5 weeks in these patients. After extra or single dose is delivered during operation, whole breast is irradiated and thus, total duration of treatment is shortened.
However, breast-conserving surgery may not be an option for some patients. If it is necessary to remove entire breast, nipple and areola can be spared to gain better cosmetic outcomes. This is called nipple- and areola-sparing surgery. Risk of recurrence in nipple and retroareolar tissue (that is located beneath the nipple) is minimized through single-dose radiotherapy for this part of breast.
After breast tumor is removed, the special applicator of the device is placed into the location of tumor for single-dose radiotherapy. However, healthy tissues are not damaged.
Do I Feel Pain During Treatment?
No. The procedure is very similar to X-ray or computerized tomography experiences.
May I Move?
No. Movement will cause deviation in target volume. However, you can breathe and swallow. You are recommended to breathe with usual rhythm or to avoid deep breathing. Your doctor will inform you about breath holding technique before the radiotherapy.
Will I Be Alone in Room During Treatment?
Yes. However, you will be continuously monitored on audiovisual screen. You can communicate with us, if you have any problem.
Will I Emit Radioactivity Throughout Treatment?
No. Radioactivity delivered for your treatment does not accumulate in your body and therefore, you do not harm loved ones and children.
May I Take Bath?
You can take shower with lukewarm water. However, wash your treatment site with baby shampoo using soft movements, but avoid rubbing. Tap dry your skin with towel and do not use hair drier. Do not rub your skin with bath glove and dry your skin gently. You may use moisturizing soap or cream that is recommended by your doctor for treatment site.
May I Take Sunbath or Swim?
It is necessary to avoid exposure to sunlight during treatment and until the skin heals. We do not recommend swimming in sea or chlorinated water during treatment. Your doctor will instruct you the correct time to swim according to your dermal findings at the end of the treatment.
How Should I Eat?
You may consult to your doctor regarding aspects of your diet that require attention according to the irradiated body part. Try to eat small servings at frequent intervals throughout your treatment. You should necessarily avoid smoking and we do not recommend regular consumption of alcohol. Your doctor will inform you about difficulty swallowing that may develop depending on the target volume of radiotherapy.
Will There Be Changes In My Skin During Treatment?
Redness, similar to sunburn, may sometimes develop on skin of the target volume. Skin may dry and redness may aggravate several weeks later. Sensitive skin may appear darker than pre-treatment skin tone at target volume of radiotherapy. However, these skin tone changes may disappear several weeks after the treatment.
In case of redness, rashes, acne, exfoliation and pus or blisters, self-medication should be avoided and it is necessary to visit a doctor or a nurse. Clothes that fit very tight to the treatment area should not be worn; the sensitive skin of treatment area should not be rubbed, brushed and scratched.
Will My Hair Fall Out?
If irradiated area covers head, scalp hair may fall out along with beard and other facial hair. Since breast radiotherapy does not target the scalp, your hair will not fall out, but armpit hair may be lost in case of axillary radiotherapy.
Can I Maintain My Sex Life?
Excluding patients who receive pelvic radiotherapy (lower abdomen and reproductive organs); other patients may resume routine sex life.
May Radiotherapy Be Repeated?
It is not recommended to repeat radiotherapy for same breast. However, a physician should decide for special circumstances.
Wrong
Women who receive radiotherapy should avoid physical contact with friends and family members, as they emit radioactivity.
Correct
X-Rays used for treatment of breast cancer do not accumulate in the body. There is no reason to avoid physical contact with people, except acting carefully to avoid a potential damage to the treatment site.
What is Lymphedema, How is It Treated?
As a result of breast cancer treatment, lymphedema may develop in arms depending on number of axillary lymph nodes dissected along with the breast.
Lymphedema is faced by one out of every four patients following treatment of breast cancer.
Initial symptoms of lymphedema manifest on proximal parts of hands and feet. Pain worsens in arms and legs. Skin of these body parts becomes tense and rough. Sensory deficit and joint stiffness may be seen in hands and feet. Strain and tenderness may develop in elbow or behind the knee.
Please click for more details on types of lymphedemas and treatment options.
Life After Breast Cancer
Diagnosis and treatment of breast cancer may cause psychological wearing and major depression in women. If psychological support is available, women may more quickly return to daily life. Diet, exercise and strict compliance to follow-up visits require attention against risk of recurrence.
Psychological Counseling in Breast Cancer
Given the fact that even being diagnosed with a simple disease impairs our daily life routines, diagnosis of breast cancer will, undoubtedly, have catastrophic psychological, social and economic effects. Being diagnosed with breast cancer for a woman means facing risk of losing economic power, job and a part of the body that creates the sexual identity as well as dysfunction of this body part or even her life.
In this regard, diagnosis of breast cancer paves the way for negative thoughts and fear in both patients and family members. On the other hand, medical technologies allow treatment of cancer and many patients regain former healthy status after treatment.
Negative thoughts arising out of diagnosis of breast cancer and ambiguity of treatment devastate existing adaptation mechanisms and cause the mechanisms to be underutilized. Future expectations and plans may be disrupted after diagnosis of breast cancer and these patients feel like they have lost power over own life. This may result in feelings such as fear, anxiety and helplessness.
You Are Diagnosed with Breast Cancer, What Will Happen?
The major fear of women with breast cancer is about metastasis or recurrence of cancer, suffering from pain and death.
Women with breast cancer go through certain psychological stages after being diagnosed and throughout the treatment. You may also proceed to these stages. Usually, the first reaction to diagnosis is “denial.” You may not believe you have been diagnosed with breast cancer, since it is truly difficult to accept you have breast cancer. Many people initially go into shock and deny diagnosis. Denial may be replaced with anger. You may find yourself constantly asking “Why me?”
You may feel angry with people around you and express fury against them. You may try to rationalize the cause and you may think “I have breast cancer, as my family distressed me too much”. Next, you may proceed to other stage that is defined as “bargaining” by experts. You may start running internal bargains and you may have certain thoughts such as “I will beat breast cancer, as I quit smoking” or “It was me who caused this disease and it is also me who will defeat it”.
Bargaining is usually followed by “depression” and “grief.” You cannot deny you have the condition after a short while once treatment is started. Surgery and treatment may start to limit your daily life. You may feel hopeless and desperate. Once this stage is done, “acceptance” starts.
You will feel neither sad nor angry at this stage. Acceptance does not mean abandoning all hopes. You will be strongly holding on to your treatment at this stage. However, it is necessary to mention that not all patients with breast cancer go through all these stages. Also, not all patients experience these stages identically.
What are Psychological Effects of Treatment Process?
All these challenging consequences of being diagnosed with cancer will be psychologically wearing and sometimes, a psychological disorder may occur. Research reports that the risk of accompanying psychological disorder is 50 percent in breast cancer. Psychological disorders that develop most commonly in breast cancer are depression and anxiety disorders.
When Should You Seek Psychological Counseling?
- If you are constantly feeling upset, anxious, sad, nervous or uneasy,
- If you believe you are unable to solve your problems,
- If you hesitate to share your problems with your physicians, family or social circle,
- If you experience difficulty in focusing your attention,
- If you cannot control your temper
We recommend you to seek counseling from a psychologist or a psychiatrist. Severing ties with life due to thoughts on your illness may affect your treatment. You should avoid taking such steps. Receiving psychological support, when required, will keep the aforementioned mood at bay.
If your finances do not allow this type of counseling, you should ask your physician all and every questions you may have, share feeling of restlessness with your physicians and all family members and loves ones and you also try to find your way out by cooperating with your physician. Sharing your problems will also alleviate your psychological stress.
What Are Benefits of Psychological Counseling?
- Increases quality of life by alleviating fear and anxiety,
- Makes you cope with your disease better and easier,
- Facilitates adaptation to your new life,
- Helps you cope with problems in various aspects of your life due to treatment and the disease,
- Guides you to see positive aspects of your life.
- Affects your physical health positively by boosting your immune system,
- Prevents risk of a more severe psychological disorder in the future, if you are at risk.
Does Your Psychology Affect Breast Cancer?
Our body is constantly communicating with our mind. Having a better mood affects our body positively. For example, if we get a headache when we are sad, we feel the ache more severely when compared to when we are happy. Thinking positively has positive effects on our immune system. However, this statement should not be misinterpreted: “I should never feel bad and I should never have negative thoughts”.
Everyone goes through bad mood with or without a cause. Nobody can constantly be very happy, anxiety-free, cheerful or energetic; therefore, you should not worry about negatively affecting your health when having bad thoughts. Minor mood swings do not affect your overall health.
Do You Have To Maintain Positive Attitude Constantly?
Thinking positively and being constantly happy do not imply believing that everything will be nice; rather, it means facing realities of your disease, understanding your options and continuing to cope with your disease. Here, it is important to minimize periods of time you feel bad and strictly focus on your disease. Try to focus on other activities, notice your negative feelings and accept and express them to help manage such periods.
You can try to maintain most part of your life as usual and even to add new elements to your life, if possible. This approach ranges from visiting a new place to new hobbies or meeting new people. Remember that new activities boost the immune system.
What Can You Gain Through Breast Cancer?
Breast cancer does not only bring negativity. You will be a stronger person while fighting this disease, even if you do not recognize it. You will have a better insight about yourself, discover ways to reach your goals, recognize your strengths, overcome your limitations, experience living the moment as well as learn to cherish every moment of life and focus on beauty in your life. You will even see your quality of life has increased and your life has been enriched, once your treatment is completed.
Loss of Breast Damages Body Image!
Breast cancer is a disease that is perceived to threaten being a woman. Removal of breast may put heavier psychological burden on women with breast cancer. Loss of breast is deemed far different from losing any other part of the body.
Loss of breast is equalized to loss of femininity, fertility, sexual attraction and sexuality. Therefore, removal of breast devastates the body image in women, self-confidence decreases and some women may experience problems with sexuality. This effect is more potent in younger women than older ones.
Suggestions to Boost Your Psychology Throughout Treatment
- Try to maintain your routine daily life as much as possible unless instructed otherwise by your physician or as long as your physical condition allows. You can prevent disruption of your social life due to your disease (work, school, etc.).
- Sharing your feelings on your disease and treatment process will help you accept your disease and will provide relief.
- You should not shy away from seeking psychological counseling, when you need it.
- Going out and being active will have positive effect.
- Occupying yourself mentally, even if not physically, will keep you from constantly focusing on your disease.
- Exercising will make you relax in physical and psychological terms and feel empowered, but intensity of exercise should be instructed by your doctor.
- Relaxation exercises and yoga will have positive effects on your psychology and body.
- Following a healthy diet will make positive contributions to your treatment.
- Communicating with other cancer patients and sharing your respective experiences with each other will help you feel better.
Diet After Breast Cancer
Eating very carefully and maintaining optimal body weight are among most important measures that should be taken to prevent breast cancer.
Correlation between breast cancer and diet is as important as it is in other cancers. Studies demonstrate that diet is effective in treatment of cancer by 30 to 40 percent. According to Data from American Institute of Cancer Research, maintenance of optimal body weight is among most important issues to prevent breast cancer. Physical activity, minimum alcohol consumption and lactation are other points…
Women with optimal body weight are known to have less risk of breast cancer in menopausal period when compared to overweight women. Moreover, weight gain increases risk of recurrence in individuals who are diagnosed with breast cancer. Sex hormones, insulin and insulin growth factor 1 in blood of obese people increase waist circumference. All these factors pose a risk regarding breast cancer.
Decrease Fat Intake
Risk of breast cancer can be reduced by limiting energy intake and maintaining ideal body fat ratio. Risk of breast cancer increases in people who consume excessive fat in post-menopausal period, as the body burns less fat. Risk is known to be lower when 20 to 25 percent of total energy intake comes from fats. The figure can increase to 30 percent in risk-free people. Diet rich in Omega-3 fat is also known to decrease risk of cancer.
Limit Alcohol Consumption
There is a correlation between alcohol consumption and breast cancer. Adequate or excessive intake of folic acid from foods, such as dark leafy vegetables (for example, spinach), liver, heart, melon, orange juice, artichoke, beet, broccoli, gombo and dry legumes is known to decrease risk of breast cancer in postmenopausal women. Alcohol consumption is known to decrease concentration of folic acid in blood and thus, risk of cancer increases. Alcohol consumption is recommended to be limited to 1 glass per day, if necessary, since drinking 3 or more glasses of alcohol per day increases risk of breast cancer.
Breastfeed
Breastfeeding decreases risk of cancer in both mother and baby. Unless there is a specific problem with development of your infant or your physician suggests otherwise, feeding only with breast milk is recommended for the first 6 months.
Which Foods Should Be Prioritized?
Green tea: The polyphenol in green tea provides protection against breast cancer. Several studies show that breast cancer is less common in people who regularly drink green tea compared to those who do not. It reduces volume of tumor cells by helping the body burn fats.
Fish: The Omega-3 fatty acid and EPA lowers cancer risk. Experts recommended eating medium-sized fish once or twice a week.
Crucifers (radish, white radish, and Russian turnip), broccoli, and Brussels sprout: They contain isothiocyanate that reduces risk of breast cancer by affect the metabolism of estrogen especially in premenopausal women. Other effective ingredients are carotenoid, isoflovan and Vitamins A, C and E that reduce the risk.
Carrot, zucchini, and cauliflower: They contain lignan that reduces risk of cancer through anti-estrogenic effect especially in postmenopausal women. They are recommended to be consumed together with foods that contain Vitamin C. Whole grain foods, sesame seed, garlic, extra virgin olive oil, apricot, peach, pear, grape, winter squash and cherry are other vegetables and fruits that are rich in lignan.
Milk and dairy: Milk, cheese, yoghurt and dairy are rich in calcium. It is known that risk of breast cancer increases in women with low calcium intake. Considering consumption of milk and dairy, it is necessary to avoid the whole ones. Low-fat or skimmed milk and dairy help both weight control and protection against cancer. Experts recommend products that contain Vitamin D in calcium intake.
There is no food that prevents development or sudden-onset of breast cancer. Although it is known that certain foods increase risk, there are studies that report contrary findings. It is widely acknowledged that consumption of vegetables decrease risk of cancer by 25 percent.
Avoid fat-rich foods after treatment. Make larger rooms for green tea, fish, crucifers, milk and dairy, carrot, broccoli, zucchini and cauliflower in your diet.
It is necessary to avoid certain foods that trigger development of cancer through negative interactions with tissues. These foods that you should remove from your table are whole-fat foods, fried meals, smoked and salted meats as well as barbecued meat.
Wrong
It is not necessary to make decision of treatment quickly and lay the burden on family members by including them in decision-making process.
Correct
Breast cancer affects the entire family. Each member of family has feelings, fears and anger that should be taken into consideration regarding this disease. The best approach is to discuss all treatment options and their effects clearly. Joint decisions may strengthen family bonds and facilitate post-treatment adaptation for everyone.
Exercise After Breast Cancer
Exercise is an essential factor for all periods of life. However, people who are operated on for breast cancer especially need exercising. These exercises aim to help the patient return to normal activities as soon as possible.
What Does Exercise Aim?
- Restoration of the erect posture.
- Eliminate stiffness in neck, low back, chest and shoulders
- Restore range-of-motion, strength and flexibility in stiff body parts
- Increase lung capacity after operation or anesthesia
- Boost cardiovascular well-being and heart-lung capacity
- Regulate blood pressure by elevating level of endorphin
- Eliminate depression, weakness and tiredness
- Prevent lymphedema by facilitating drainage of lymph fluid
- Prevent scar formation
- Avoid from frozen shoulder
- Most importantly, boost fighting spirit of patient
What Should Be Gradually Done For Exercise After Operation?
Rehabilitation should be started as soon as possible to strengthen weak muscle groups that have lost flexibility after surgery and to help flexibility and strength of affected joints. Rehabilitation focuses on muscles of shoulders, neck, chest, back and rotator cuff in the initial phase, while abdomen, low back and legs are prioritized in subsequent stages.
Posture muscles are trained again to correct posture disorders and ensure more appropriate body posture. Involved muscles are trained again to restore safer mobility of patients. Deep breathing is trained by rehabilitating muscles of chest, rib cage and back and thus, diaphragm and lungs gain more room for movement. Efforts are made to increase physical and general condition in order to accelerate postoperative convalescence and to tolerate chemotherapy and radiotherapy better.
Another important target of these exercises is to reduce weight gain during and after chemotherapy, radiotherapy or menopause, increase strength and boost or maintain fitness, body composition and bone density. Thus, individual can recognize own power and feel well.
Physical condition and healing periods are not same for everybody. Therefore, patients are evaluated in all phases of the program in order to create personalized plans. Exercises are always started with easy moves with minimal repeats. Next, they are gradually increased. Too quick advancement may result in injury and sickness. It is necessary to contact the physician who planned the program, if even minor problem is faced.
What Should Be Taken Into Consideration In Rehabilitation?
It is necessary to mobilize as earlier as possible after surgery. However, sudden and quick moves should be avoided.
- Arm should be elevated and supported with 2 pillows while lying or sitting in order to prevent swelling of arm after the surgery.
- Stretching exercise should be done several times a day for both halves of the trunk and each move should be repeated for 3 to 5 times.
- If pain and tiredness persist, it is wise to rest.
- Walking at short distances for several minutes twice of thrice a day may even restore strength after surgery.
- Lifting objects heavier than 1 to 1.5 kg should be avoided in early postoperative period especially by the affected arm.
- One should act carefully in order not to carry any object heavier than 2.5 kg in the long term in order to prevent swelling in arm.
- Shoulder bags should not be used, because shoulders straps may cause lymphedema by exerting pressure on shoulder.
- One should be sure that postoperative swelling regressed and surgical wounds completely healed before starting active exercise.
- One should focus on native rhythm of body and track own insight.
- In case of suspicion, one should consult to primary doctor, nurse or physiotherapist.
- It is necessary to make efforts every day even for a minor improvement. Being self-assertive is very crucial for improvement.
If An Abdominal Muscles Is Used For Cosmetic Procedure;
- Pushing moves and activities over the head should be avoided in the early period.
- Abdominal and lumbar exercises can be started 10 weeks after surgery. Spine should be stabilized by placing a thin support beneath the hip during these exercises and excessive load should not be born on the spine.
- Exercises should be done slowly and smoothly to avoid tiredness and dizziness, f the blood count is low.
- Safest ones are condition exercises that include walking and cycling in this period.
- Quality of the exercise is more important that the quantity. When it is done right, it provides more benefit even in lower numbers.
Generally, long-term programs that are modified for each stage are recommended for patients who are undergone breast surgery. Program is planned in accordance with physical characteristics, duration of healing, type and complexity of surgery, co-existing systemic problems, and additional treatments such as chemotherapy and radiotherapy.
Disease-specific exercises are combined with those which strengthen muscles of abdomen and legs and stabilize the spine. These are followed by aerobic and strengthening exercises that aim to boost endurance, speed the metabolism, increase muscle fitness and bone density and to improve body composition.
Pain, numbness, stiffness, restricted movement, strength loss and swelling are most common musculoskeletal problems that are faced after breast cancer surgery.
Physical condition and recovery periods are different for every patient. Therefore, these exercise programs are personalized for each patient.
What are Stages of Exercise Program?
Stage 1: Early postoperative period. It is necessary to start basic exercises following surgery to decrease swelling, alleviate pain and tenderness and to achieve physical and mental recovery. Programs generally start with light stretching and strengthening exercises. The exercises should be performed smoothly and gently in several repeats twice or thrice a day. Deep breath exercises should be remembered to decrease pain and tension. These exercises are started as soon as possible after the surgery. Following moves are recommended for this period:
- It is wise to start with extending and flexing the elbow, rotating the wrists and opening and closing fists. Swelling regresses, if these moves are repeated several times throughout the day.
- They are continued in sets of 2 after they are performed easily and safely. One should rest after each set.
- Exercise session should not be prolonged in early postoperative period; it is wise to repeat moves several times in the day time.
- Upper extremity exercises should be performed in maximum 3 sets with 10 repeats.
- Program should always include mild warm up before the exercise and mild stretching after the exercise.
- Arms should be elevated above level of heart using pillows at night.
- It is necessary to walk short distances every day.
Stage 2 : This period covers an interval up to 6 weeks after surgery. Slow and controlled movements prevent weakness and loss of flexibility in arms. Following moves are recommended for this period:
- Deep breathing exercises have a great role in this period as they alleviate pain and ensure relaxation along with relief of spasm in muscles of back and chest.
- Walking slowly at frequent intervals increases endurance and prevents muscle atrophy.
- Warm up before exercise and stretching movements afterwards are necessary.
- Duration of walk can be prolonged in this period.
- Resistance band exercises can be started, after surgical wounds heal.
Stage 3: This period of time extends from 6 weeks to 10 weeks after surgery. It covers more advanced upper body exercises. Leg movements can also be started, when full recovery is achieved. Following moves are recommended for this period:
- It is rationale to start more active walks.
- Stationary bicycle and swimming are recommended to be started 6 weeks after surgery for arm and shoulder health.
- Frog style swimming is recommended in the early period. Free style and backstroke swimming should be avoided for 2 months after the surgery.
- Butterfly style should also be avoided, if lymph node is dissected or an implant is placed.
- Pilate’s ball, resistance bands and small weights can be used in this period.
- These exercises are decided in accordance with patient’s overall health and past experience of exercise.
Stage 4: This stage extends to >10 weeks after surgery and covers more active aerobic (endurance) activities. Exercises such as moderate-intensity walking, stationary bicycle and ascending stairs slowly can be started at this period. This stage focuses on increasing strength and flexibility. It is maintained with aerobic, strengthening and flexibility exercises in the long term. Jogging program is maintained. Patients should be evaluated by primary doctor before proceeding to advanced exercise program. Pilates ball, resistance bands and small weights can also be used in this period.
Follow-up After Breast Cancer
Patients should be followed up through detailed health assessments in first 3 years after treatment of breast cancer.
Breast cancer relapses locally – at the surgical site- by 30 percent and in distant organs by 70 percent. Recurrence generally occurs within the first 3 years. Therefore, it is necessary to follow up patients very closely especially in the first three years. Follow-up visits are generally scheduled as follows: At 3-month intervals in the first three years, semi-annually in subsequent two years and annually beyond five years.
Which Examinations Are Ordered?
Whole body bone scan, chest (PA) X-ray, liver ultrasound and various tumor markers as well as alkaline phosphatase are analyzed at certain intervals in patients with breast cancer and results are recorded for future comparisons. Tomography of Thorax and Abdomen, plan roentgenograms in case of bone ache and MRI may be ordered along with general body scan, such as PET-CT, if required.
What should be taken into account?
Complaints of patients are assessed and detailed evaluations are made in follow-up visits. Examinations are considered unnecessary for patients with no complaint or suspicious finding. However, detailed examinations are planned for patients with any suspicious finding to investigate the underlying cause. First mammography is scanned 4 to 6 months after radiotherapy in patients who are undergone breast-conserving surgery and it is repeated annually. Annual radiologic examinations are necessary for those who underwent mastectomy.
Given the risk of relapse of breast cancer, patients should be followed up after treatment. Follow-up visits should be scheduled at quarter intervals in the first three years, semiannually in subsequent two years and annually beyond five years.
Wrong
Women with past history of breast cancer should have bone scan, CT, blood tests and X-ray every year.
Correct
These additional tests might be required in some cases. Routine physical examination and mammography at annual intervals is recommended for women who are healthy without relapse for at least 5 years. In case of radiotherapy, chest X-ray can be ordered every year.
Breast cancer is the most common type of cancer in women and one out of approximately eight women is diagnosed with breast cancer in her lifetime. However, chance of cure is almost 100 percent, if breast cancer is detected in early stage.
Meme Kanseri Ne Kadar Süre Hiç Belirti Vermeden İlerleyebilir?
Acıbadem Maslak ve Bakırköy Hospital, Genel Cerrahi Uzmanı Prof. Dr. Cihan Uras, Kanser üzerine soruları yanıtlıyor.Self-examination at monthly intervals in every woman older than 20, clinical examination once a year and certain imaging techniques play a very crucial role in early diagnosis. Self-examination of breasts is done in days following termination of menstrual cycle and in any day of the month in postmenopausal women.
Clinical examination should be done once a year by a doctor who is specialized in breast in women older than 40. It can be started before 40, if person has family history of breast cancer. Mammography is usually started after 40, but it can be recommended at younger ages depending on family history.
Men can also be diagnosed with breast cancer and therefore, all men, especially ones with risk factors, should pay maximum attention to changes in their breasts. Screening methods facilitate early diagnosis of breast cancer and thus, this disease can be completely cured in women.
Meme Kanserinin Erken Teşhisi İçin Önerilen Testler Nelerdir?
Acıbadem Altunizade Hospital Onkoloji Uzmanı, Prof. Dr. Başak Oyan Uluç, "Kanser Tarama Testleri" üzerine soruları cevaplıyor.Breast cancer begins in milk gland or cells that line the canals, which flow breast milk to the nipple. Although the exact cause is yet unknown, gene mutations that lead to genetic predisposition increase the risk of breast cancer.
Breast cancer is a tumor that develops secondary to uncontrolled growth of cells with potential of spread to other organs due to various factors in milk glands and the cells that line the milk ducts, which flow the breast milk to the nipple.
Causative factors of breast cancer are not clearly known. However, some factors that are more likely to play a role have been identified in studies that have been conducted to date. Gene mutations (abnormalities of genes that make a person more prone to cancer) that lead to genetic predisposition increase risk of cancer in some women, while no risk factor other than being a woman can be detected in others.
Northern European Women Are At Highest Risk
Rate of deaths secondary to breast cancer is high in countries of Northern Europe. The rate is 22.6/100 thousand in these countries. On the contrary to Northern European women, breast cancer-deaths are at lowest rate in Chinese and Japanese. The figure is 5.6/100 thousand in China and 8.3 in Japan.
One in every 8 women in the U.S. is diagnosed with breast cancer during her lifetime. More than 182 thousand women were diagnosed with breast cancer in the U.S. in 2008. Approximately 40 thousand women died due to breast cancer. However, there are also promising results to offset these upsetting statistics.
Today, 2.5 million healthy survivors of breast cancer live in the U.S. It is believed that increased awareness of mammographic screening in women over 40 years of age and constant decline in hormone replacement therapies recommended for menopausal women have boosted the success of treatment in breast cancer.
What are Symptoms of Breast Cancer?
It takes a long time to detect conversion of a cell into a cancerous form or development of a tumor in breast tissue in a clinical examination or an imaging study. Women can generally notice a lump, measuring approximately 1 cm in size, in self-examination of breasts.
Today, symptoms of breast cancer are usually first noticed by women. Cancerous lesions are rather solid lumps with sharp margins and rough surface and they are usually firmly adhering to the origin in breast tissue. If cancer has already metastasized to distant organs, metastasis may rarely be the initial sign of breast cancer. Breast cancer often prefers hip bones, vertebrae, lungs and liver to metastasize.
Meme Kanseri Ne Gibi Belirtiler Verir?
Acıbadem Maslak ve Bakırköy Hospital, Genel Cerrahi Uzmanı Prof. Dr. Cihan Uras, Kanser üzerine soruları yanıtlıyor.However, some patients do not show any symptoms of breast cancer and it can be detected only in a mammography scan. One should immediately visit a doctor, if at least one of following symptoms is recognized.
- A palpable mass (solid lesion, lump) in breast or arm pits
- Nipple discharge (bloody or clear fluid from single duct)
- Retraction, inversion or deformity in nipple
- Changes in nipple skin (exfoliation, crusting)
- Sore or redness in skin of breast
- Edema, swelling or retractions on skin of breast (orange peel sign)
- Growth, deformity, asymmetry or discoloration of skin in breast (redness, etc.)değişiklik (kızarıklık vs.)
Breast cancer gets the second rank among all cancer deaths. Lung cancer occupies the first line. According to Year 2007 data of Turkish Statistics Institute (TUIK), 22 out of every 100 thousand women are diagnosed with breast cancer in our country with a total population of 70 million people. Reported mortality rate of breast cancer is approximately 10/100 thousand women.
Stages of Breast Cancer
Breast cancer is staged according to size of tumor, spread to lymph nodes in arm pits or metastasis to distant organs. Stage 0 implies “in situ” period, where the cancer does not pose risk of metastasis or spread. In the next stage (stage I), tumor measures smaller than 2 cm in size and it has not yet spread to lymph nodes. In stage II, tumor is smaller or larger than 2 cm, but its spread to lymph node is likely. In stage III, dimensions increase and tumor has spread to axillary lymph node(s). In stage IV, distant organs, such as breast, armpit, lung, heart, liver and brain, have been involved by cancer.
Treatment of Breast Cancer
In breast cancer, success of treatment correlates to how early the diagnosis is made. Surgical treatment accounts for a significant part of the treatment in breast cancer. Non-surgical treatment options (chemotherapy, hormone therapy, radiotherapy) intend to prevent relapse of tumor or metastasis to other organs.
How Is Breast Cancer Detected?
While breast cancer does not cause any symptoms in some patients, it is usually noticed when a solid lump is palpated in breast. Breast cancer is most commonly detected in self-examination of breasts or mammography and ultrasound screening. The lump is the most common complaint and the mostly noticed sign of breast cancer.
So, how is breast cancer noticed? Bloody nipple discharge, inversion or collapse on skin of breast and retraction or orange peel sign are the leading heralds for breast cancer. Moreover, sudden-onset redness, swelling and asymmetrical growth can also be seen. Another prominent symptom is crusting in nipple, leading to an eczematous appearance.
Breast cancer typically does not cause any pain. Women may notice the aforementioned symptoms in self-examination. However, patients may visit a doctor with complaint of pain at a location close to breasts. For such cases, your doctor may advise you a mammography screening.
One out of every eight women is diagnosed with breast cancer, which has constantly increasing incidence, in our country, as is the case with all other countries. On the other hand, new treatment options are recently developed to fight the disease thanks to technological advances in medicine. Women with breast cancer can beat the cancer, if it is diagnosed at early stage and the condition is managed with appropriate treatments. Therefore, it is crucial for women to perform self-examination one week after menstrual cycles.
Risk Factors of Breast Cancer
Cender
Breast cancer is most commonly diagnosed in women. Its incidence rate is less than 1% in men..
Age
Breast cancer is largely detected above 50 years of age. The incidence is low below 35. Incidence of breast cancer was 25/100 thousand in American women at age range of 30 to 34 years in 2000 to 2004, but the figure increases to 190/100 thousand at age range of 45 to 49 years and 455/100 thousand at age range of 70 to 74 years.
Hereditary breast cancer or breast cancers secondary to genetic disorders are more common in young women.
Family History
History of breast cancer particularly in 1st degree maternal relatives (mother, maternal aunt, grandmother, and daughter) is deemed a critical risk factor. Premenopausal onset of breast cancer and/or bilateral breast cancer in these relatives increases the risk further.
Estrogen Hormone
Earlier menarche (for example before 12) and later menopause (for example at the age of 55) increase the risk of breast cancer proportionally. It is believed that use of birth control pills also increase the risk of breast cancer, albeit very slightly.
Post-menopausal Hormone Therapy
Combined hormone medications which contain estrogen and medroxyprogesteron acetate and are prescribed for long-term use (5 years or more) by gynecologists to prevent hot flashes and similar problems of menopause increase the risk of breast cancer more significantly in comparison to medicines which contain only estrogen.
Past History of Breast Biopsy
Risk of breast cancer is increased 1.5 to 2 folds (mild) by moderate hyperplasia that is detected in breast biopsies or 3 to 5 folds (moderate) by atypical ductal hyperplasia, while lobular carcinoma in situ (without metastasis) and atypical ductal hyperplasia or lobular hyperplasia combined with positive family history increase the risk by 8 to 10 times (high).
History of Breast Cancer
Past history of breast cancer in one breast of woman increases the risk of breast cancer in other breast approximately by 2 folds.
Radiotherapy
Incidence of breast cancer increases in people with past history of chest radiotherapy for other cancers (lymphoma etc.) in childhood.
Nutrition and Environmental Factors
Having a diet rich in fat and weight gain increase the risk of breast cancer, especially in menopausal women. Consumption of alcohol (more than a glass per day) also increases the risk, while effects of smoking are still debated. It is also known that regular exercise and physical activity decrease the risk of breast cancer.
Genetic disorders
Hereditary breast cancer genes (BRCA1 and BRCA2) account for 5 to 10 percent of all breast cancers.
Wrong
An individual has no risk of cancer, if there is no family history of breast cancer.
Correct
Family history is negative in 75% of women with breast cancer. Being a “woman” is anyway a risk factor for breast cancer.
What are Types of Breast Cancer?
There are various types of breast cancer. However, they are broadly classified into two groups; the first one covers non-invasive or in situ cancers, while the second group contains invasive ones.
Meme Kanseri Tipleri Nelerdir?
Acıbadem Taksim Hospital doktorlarından; Genel Cerrahi Uzmanı Doç. Dr. Tamer Karşıdağ "Meme Kanseri" üzerine soruları yanıtlıyor.Non-Invasive Cancers
Non-invasive (in situ) cancers are divided into two subgroups; ‘ductal carcinoma in situ’ and ‘lobular carcinoma in situ’. Detection rates of non-invasive (in-situ) cancers in all biopsies increased from 1.4 percent to 10 percent and their share among all cancers increased from 5 percent to 15 percent, when screening mammography had been more widely used especially after 1980s.
Classic lobular carcinoma in situ: this is a critical sign which increases the risk of breast cancer by 8-10 folds. These patients can be prescribed certain preventive medicines along with close follow-up or preventive simple mastectomy (removal of bilateral breast tissue) can be performed. Promising cosmetic outcomes can be obtained, when they are combined with plastic surgery and reconstructive surgery procedures, such as prosthesis.
In situ ductal cancers (ISDC, intraductal cancers): These are not generally noticed in examinations. They are manifested by irregular small calcium deposits that are visualized in mammography (pleomorphic microcalcification) and/or bloody/clear nipple discharge from a single duct. ISDC is deemed a phase of transition from healthy cells into cancerous cells that have potential of metastasis (invasive). Since they do not cause a lump, they are marked with a wire or a radioactive substance and removed.
If the breast cancer involves only one focus, a sufficient large safety zone of healthy tissues is left around the cancer. The disease follows a clinically favorable course, when the rest breast tissue is irradiated (radiotherapy).
If the breast tissue is diffusely involved, it is necessary to remove breast tissue completely (simple mastectomy) and in this case, rate of cure is almost 100 percent. Involvement of axillary lymph nodes is rare in pure ISDC (1 to 3 percent). Therefore, it may be required to remove sentinel lymph nodes that are located in arm pits and most likely to catch cancerous cells in certain aggressive cancers (high grade etc.), if the breast will be entirely removed.
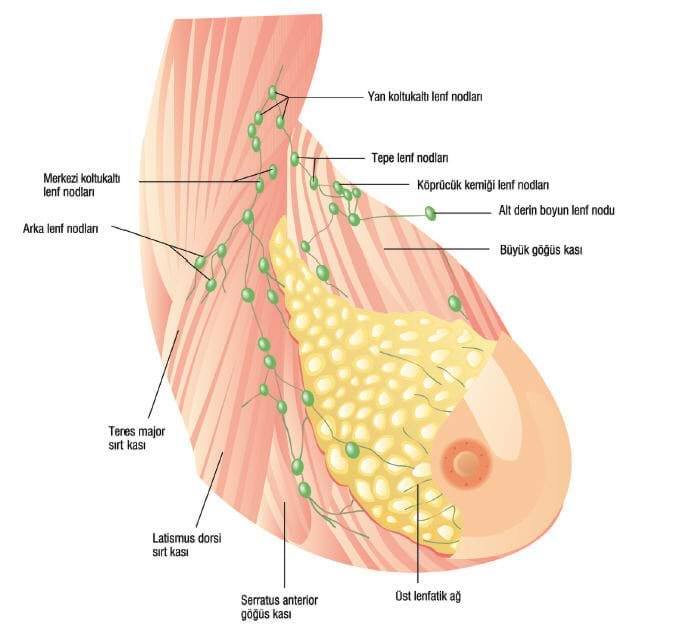
Invasive Cancers
Ductal carcinoma that begins in cells, which line the milk ducts that flow milk to the nipple, is the most common type of breast cancers. This is also divided into subgroups according to invasion: Ductal carcinoma is called in situ if it is not likely to invade or otherwise, it is invasive due to potential of metastasis.
Lobular carcinoma refers to the cancer that begins in lobules – the glands that produce milk. Lobular carcinoma is also divided into two subgroups according to invasion. In situ form implies absence of invasion, while invasive form refers to potential of metastasis.
Hereditary Breast Cancers
Causes?
Hereditary (genetic or familial) breast cancer syndromes are seen only in 5-10 percent of the breast cancer patients. There are 2 genes which are responsible for 80% of hereditary breast cancer cases: BRCA-1 and BRCA-2. Women with mutation in BRCA-1 gene are at risk of breast cancer by 85 percent and ovarian cancer by 45 percent before the age of 70. For carriers of BRCA-2 gene mutation, the risk of breast cancer and ovarian cancer is 84 percent and 76 percent, respectively, until they are 70.
How is it diagnosed?
Genetic tests are required to identify BRCA-1 and BRCA-2 mutations. For this group of patients, self-examination of breasts should be started at 18 years of age, while mammography, semi-annual or annual clinical breast examination and annual breast MRI are recommended at 25 to 35 years of age. Moreover, these individuals should not ignore ovarian cancer screening at semi-annual intervals, starting when they are 30 to 35 years old.
Which Measures Are Taken?
For these people, primary risk-reduction methods are use of medications that suppress estrogen and risk-reduction preventive surgery. These surgical interventions include removal of bilateral ovaries and breasts (bilateral salpingo-oopherectomy and prophylactic bilateral mastectomy). Preventive removal of ovaries decreases the risk of breast cancer by 50%, while prophylactic mastectomy reduces the risk by 90%.
Kalıtsal Meme Kanseri İçin Hangi Önlemler Alınabilir?
Acıbadem Taksim Hospital doktorlarından; Genel Cerrahi Uzmanı Doç. Dr. Tamer Karşıdağ "Meme Kanseri" üzerine soruları yanıtlıyor.Genetic counseling is a must for Ashkenazi women with Eastern and Middle European origin particularly if they are a first-degree one or more than one relative with young-onset breast cancer or bilateral breast cancer, as incidence of hereditary cancers is high in this population. Genetic counselors inform individuals, who carry these risks, about necessity of BRCA-1 and BRCA-2 gene mutation tests by evaluating them from medical and psychosocial aspects.
Who are at risk?
Family history of breast cancer in one or more than one 1st and 2nd degree relatives suggests a hereditary breast cancer. Moreover, co-existence of breast cancer and ovarian cancer in young women, who are 20 to 30 years old, is also suggestive of hereditary breast cancer. Family history of breast cancer in mother or sister is deemed critical risk factor.
Breast Cancer in Pregnancy
Breast cancer is the most common type of cancer in pregnant and lactating women. Studies report that breast cancer develops in 2 to 4 out of every 1000 pregnancies. Pregnancy may cause delay in diagnosis of cancer in such patients. Because physiological changes in breast may misguide patients and physicians. Therefore, when diagnosis is made, cancer has already invaded axillary lymph nodes more intensively..
What Are Diagnosis Methods?
Ultrasound is the first diagnostic device to consider, if a suspicious finding is detected in examination. Core needle biopsy should be preferred for diagnosis.
As patients can be anesthetized safely in weeks 14-36 of pregnancy, surgical procedures can be carried out. However, it can be postponed if there are 3 to 4 weeks to the delivery or delivery can be induced 1 to 2 weeks earlier.
Use of blue dye for sentinel lymph node biopsies is not recommended in pregnancy, unless invasion of cancer to axillary lymph nodes is detected in examination.
Although gamma probe-guided sentinel lymph node biopsy with low-dose radioactive agent injection is used for a few patients and considered safe in pregnancy, they are not recommended before Week 30. It is advised to avoid these practices, until more evidence is obtained about their side effects.
How Is Breast Cancer In Pregnant Patients Treated?
In pregnancy, modified radical mastectomy which implies total removal of breast along with dissection of axillary lymph nodes is commonly preferred as standard surgery technique.
Chest wall or breast is not irradiated in pregnancy. Therefore, breast-sparing surgery can be considered only at terminal stages of pregnancy in order not the delay radiotherapy or otherwise, radiotherapy is postponed until delivery.
In the first 13 weeks, it is better to terminate pregnancy, as chemotherapy induces toxic effect on fetus and causes miscarriage.
Risk of fetal anomalies due to chemotherapy is 1.3 percent as of week 14. This rate is equal for a fetus that is not exposed to chemotherapy, which means that some chemotherapeutic agents like anthracycline (doxorubicin) can be safely used for pregnant patients.
Generally, it is accepted that chemotherapy can be used until week 35, but it should be paused 3 weeks before delivery to prevent potential resultant problems, as blood parameters of mother can be affected adversely.
Use of tamoxifen is also not recommended in pregnancy and it is postponed until delivery.
To prevent exposure of newborn infants to all chemotherapeutic agents or tamoxifen through breast milk, lactation is suppressed with medicines.
Women with breast cancer are advised to consult their physicians regarding future conceptions. Usually, a new pregnancy is not allowed for 5 years in women with stage II-III cancers. A patient with stage I cancer should wait for at least two years, unless tamoxifen is used.
Breast Cancer in Men
Although breast cancer is most commonly detected in women, it is also a problem for a very small group of men. Less than 1 percent of breast cancers are detected in men. Family history of breast cancer in 30 percent of male patients is a very notable factor. It is considered that BRCA-2 genes play a role in development of breast cancer in a part of men.
Erkeklerde Meme Kanseri Ne Gibi Belirtiler Verir?
Acıbadem Maslak ve Bakırköy Hospital, Genel Cerrahi Uzmanı Prof. Dr. Cihan Uras, kanser üzerine soruları yanıtlıyor.What Are Risk Factors?
Most of these cancers develop at and after 60 years of age. Undescended testes, testicular trauma, surgical removal of testis (orchiectomy) and use of estrogen hormone are acknowledged risk factors. When tumors of these patients are examined, estrogen and progesterone receptors are identified in at least 75 percent of cases, but c-erbB-2 protein is rather rare.
Erkekte Meme Büyümesinin Nedenleri Nelerdir?
Acıbadem International Hospital, Endokrinoloji ve Metabolizma Hastalıkları Uzmanı Dr. Bilge Ceydilek; "Erkeklerde Meme Büyümesi (Jinekomasti)" üzerine soruları cevaplıyor.What Are Symptoms?
Almost all patients complain of a lump behind the areola, also including nipple. On the contrary to gynecomastia (enlargement of breast in men), this pain-free solid lump with irregular margins is located at only a part of the areola and clear or blood nipple discharge is noted in 80 percent of patients.
How Is It Treated?
Today, modified radical mastectomy is the technique of choice for these patients. Breast-sparing surgeries are not appropriate to remove large tumors, while more studies are warranted for sentinel lymph node dissections due to low number of patients.
Treatment may involve chest wall radiotherapy depending on involvement of axillary lymph nodes, while tamoxifen is preferred for estrogen receptor-positive cases and chemotherapy protocols that contain taxane and/or anthracycline can be considered depending on invasion of axillary lymph nodes.
Inflammatory Breast Cancer
Inflammatory breast cancer is deemed most aggressive type of breast cancer with poorest prognosis. It can be confused with inflammatory breast diseases that completely involve the breast. It progresses with redness and hardness without any sign of mass lesion. In case of inflammatory breast diseases that persist despite antibiotherapy, breast cancer should be suspected and biopsy should be performed.
What is Function of Breast?
It is necessary to take nipple discharge, breast pain and palpation of lump in self-examination seriously and visit a doctor. These signs do not always imply a cancer. Although cancer is detected in some patients in the light of examination, others are mostly diagnosed with benign breast diseases.
Function of Breast
A breast consists of milk glands, milk ducts that flow milk to the nipple and adipose and connective tissues that fill the spaces between glands and ducts. Each breast is located in front of chest muscles over ribs. Nipple is located at the central zone of the areola. There are also lymph channels, where a colorless fluid, called lymph, flows, in breasts. Lymph channels drain into small round lymph nodes.
Lymph node groups of breast are primarily located in armpit, immediately above the clavicle and nearby the sternum (chest bone). Lymph nodes filter and catch bacteria, cancerous cells and other hazardous compounds that can be found in lymph system.
Nipple Discharge
Bloody or clear fluids draining from single breast and single channel form the nipple discharges that require investigation to determine the underlying cause. In this case, you need to visit your doctor immediately. Mammography is scanned along with ultrasound in patients older than 35. Findings of clinical examination and imaging techniques, such as mammography and ultrasound, can be unremarkable. Magnetic resonance imaging and/or ductography can also be considered, if required.
Recently, a thin device (<1 mm) equipped with a light (ductoscope) is inserted into the draining channel of the nipple to investigate if there is a lesion in the duct. Intraductal papilloma, a benign lesion that increases the risk of breast cancer, is detected in two thirds of nipple discharges, but the second most common finding is cancer.
Discharge of milk-colored or green fluid from nipple of both breasts and/or multiple ducts in response to massage or compression may be a totally normal condition. Gray to green fluid drains from multiple ducts in response to pressure in cystic formations of breast.
Discharge of milk-colored or green fluid from both breasts or multiple ducts in one breast are deemed benign signs. In such cases, ultrasound can be scanned depending on age of patient (<35-40 years), if normal findings are detected in clinical examination, and the patient is placed on follow-up, if results are normal. Patients are recommended not to squeeze nipple in order not to provoke discharge.
Breast Pain
Breast pain (mastalgia) is among most common complaints in women. The most common form is characterized by pain, tenderness and swelling that begin 2 weeks before menstrual cycle and regress when the period starts.
Breast pain that is not linked to menstrual periods can be secondary to past history of breast surgery, pain radiating from muscles of chest wall or neck, hormonal fluctuations, psychological causes, caffeine intake and insufficient intake of important fatty acids in diet
Memede Ağrı Neden Olur, Kanser Belirtisi Olabilir Mi?
Acıbadem Bursa Hospital Genel Cerrahi Uzmanı, Dr. Volkan Tümay; "İyi Huylu Meme Hastalıkları" üzerine soruları cevaplıyor.Benign Breast Lesions
Most common breast lesions are listed below:
- Cysts (filled with fluid)
- Fibroadenoma
- Phyllodes
Other solid benign lesions: Radial scar and complex sclerosing lesions, papilloma, lipoma, hamartoma, fat necrosis, leiomyoma, granular cell tumors etc.
Cysts in Breast
Cysts are sacs that are filled with fluid and they are secondary to dilatation of milk glands. It is detected in one out of 14 women and it is common in the age range of 40 to 49 years. Generally, it accounts for 25 percent of breast lesions. One fifth of cysts are larger than 1 cm and there are multiple cysts in half of cases. Galactocele, cysts filled with breast milk, can be detected in lactating mothers.
Fibroadenoma
It is the most common type of benign breast tumor in women. Usually, a solitary lesion is detected in young women in the age range of 20 to 30 years. Ten to fifteen percent of patients have more than one lesion. Simple fibroadenomas account for two thirds of fibroadenomas and they do not increase risk of cancer, if there is no other risk factor (such as family history).
Phyllodes Tumor
It accounts for less than 1 percent of all breast tumors. It can be clinically confused with giant fibroadenoma. It can be differentiated from giant fibroadenomas through pathological characteristics, clinical recurrence and spread to other organs. It is extremely difficult to differentiate phyllodes tumor from fibroadenoma with ultrasound, mammography and magnetic resonance imaging. Core needle biopsy can be considered, but it may not be safe. Final differential diagnosis should be based on examination of surgically removed lesion by a pathologist.
The principal treatment option of Phyllodes tumor is surgical removal of the lesion. If sufficient breast tissue can be spared in cosmetic terms, breast-conserving surgery can be carried out by leaving a safe zone (1-2 cm). If tumor involves entire breast (such as a tumor measuring 20 cm in size), oncologic approach should be total removal of breast. After breast is removed, an implant can be placed by plastic surgeon in the same session. Phyllodes tumors do not spread to axillary lymph nodes.
Therefore, axillary lymph nodes are not touched. Local recurrence is very likely in breast and it spreads to lungs. Overall five-year survival rate is 91% for benign phyllodes and 82% for malignant phyllodes. Surgery is the only treatment option for benign phyllodes. Chest wall radiotherapy and chemotherapy can be prescribed for only a part of malignant cases. Generally, role of these adjunctive treatments is debated following sufficient surgical treatment.
What Is Intraductal Papilloma?
Intraductal papilloma may begin in milk ducts located beneath the nipple or lateral parts of breast. It is the most common underlying cause of bloody nipple discharge and it is diagnosed in the age range of 30 to 50 years. These tumors that measure <1 cm or 3 to 4 mm in size are usually located in the milk duct.
Papillomas that begin at lateral parts of breast are more common in young women and they are less likely to be accompanied by nipple discharge. The risk of cancer in both breasts is higher for multiple intraductal papillomas that are visible on skin of breast than single intraductal papilloma that begins in the nipple.
Inflammatory Diseases of Breast (Mastitis)
Inflammatory diseases of breast (mastitis) are diagnosed at range of 18 years to 50 years. In case of abscess (pus), it should be immediately drained through a surgical procedure. It may be clinically difficult to differentiate from breast cancer. For cases that do not respond to antibiotherapy, biopsy is a must to rule out cancer in infections.
Doctors
-
![Prof. ABDULLAH ZORLUOĞLU, M.D.]() Prof. ABDULLAH ZORLUOĞLU, M.D.
General Surgery
Book an Appointment
Prof. ABDULLAH ZORLUOĞLU, M.D.
General Surgery
Book an Appointment
-
![Prof. BÜLENT SAÇAK, M.D.]() Prof. BÜLENT SAÇAK, M.D.
Aesthetic, Plastic and Reconstructive Surgery
Book an Appointment
Prof. BÜLENT SAÇAK, M.D.
Aesthetic, Plastic and Reconstructive Surgery
Book an Appointment
-
![Prof. CAN KÜÇÜK, M.D.]() Prof. CAN KÜÇÜK, M.D.
General Surgery
Book an Appointment
Prof. CAN KÜÇÜK, M.D.
General Surgery
Book an Appointment
-
![Prof. CİHAN URAS, M.D.]() Prof. CİHAN URAS, M.D.
General Surgery
Book an Appointment
Prof. CİHAN URAS, M.D.
General Surgery
Book an Appointment
-
![Prof. ERKİN ARIBAL, M.D.]() Prof. ERKİN ARIBAL, M.D.
Radiology
Book an Appointment
Prof. ERKİN ARIBAL, M.D.
Radiology
Book an Appointment
-
![Prof. FÜSUN TAŞKIN, M.D.]() Prof. FÜSUN TAŞKIN, M.D.
Radiology
Book an Appointment
Prof. FÜSUN TAŞKIN, M.D.
Radiology
Book an Appointment
-
![Prof. GÜL ESEN İÇTEN, M.D.]() Prof. GÜL ESEN İÇTEN, M.D.
Radiology
Book an Appointment
Prof. GÜL ESEN İÇTEN, M.D.
Radiology
Book an Appointment
-
![Prof. GÜL BAŞARAN, M.D.]() Prof. GÜL BAŞARAN, M.D.
Oncology
Book an Appointment
Prof. GÜL BAŞARAN, M.D.
Oncology
Book an Appointment
-
![Prof. HİLAL ÜNAL, M.D.]() Prof. HİLAL ÜNAL, M.D.
General Surgery
Book an Appointment
Prof. HİLAL ÜNAL, M.D.
General Surgery
Book an Appointment
-
![Prof. MELİH PAKSOY, M.D.]() Prof. MELİH PAKSOY, M.D.
General Surgery
Book an Appointment
Prof. MELİH PAKSOY, M.D.
General Surgery
Book an Appointment
-
![Prof. MERİÇ ŞENGÖZ, M.D.]() Prof. MERİÇ ŞENGÖZ, M.D.
Radiation Oncology
Book an Appointment
Prof. MERİÇ ŞENGÖZ, M.D.
Radiation Oncology
Book an Appointment
-
 Prof. METİN ERTEM, M.D.
General Surgery
Book an Appointment
Prof. METİN ERTEM, M.D.
General Surgery
Book an Appointment
-
![Prof. METİN ÇAKMAKÇI, M.D.]() Prof. METİN ÇAKMAKÇI, M.D.
General Surgery
Book an Appointment
Prof. METİN ÇAKMAKÇI, M.D.
General Surgery
Book an Appointment
-
![Prof. NURAN BEŞE, M.D.]() Prof. NURAN BEŞE, M.D.
Radiation Oncology
Book an Appointment
Prof. NURAN BEŞE, M.D.
Radiation Oncology
Book an Appointment
-
![Prof. ORHAN DEMİRCAN, M.D.]() Prof. ORHAN DEMİRCAN, M.D.
General Surgery
Book an Appointment
Prof. ORHAN DEMİRCAN, M.D.
General Surgery
Book an Appointment
-
![Prof. ÖZGE GÜMÜŞAY, M.D.]() Prof. ÖZGE GÜMÜŞAY, M.D.
Oncology
Book an Appointment
Prof. ÖZGE GÜMÜŞAY, M.D.
Oncology
Book an Appointment
-
![Prof. ÖZLEM SÖNMEZ, M.D.]() Prof. ÖZLEM SÖNMEZ, M.D.
Internal Medicine
Book an Appointment
Prof. ÖZLEM SÖNMEZ, M.D.
Internal Medicine
Book an Appointment
-
![Prof. ŞÜKRÜ AKTAN, M.D.]() Prof. ŞÜKRÜ AKTAN, M.D.
General Surgery
Book an Appointment
Prof. ŞÜKRÜ AKTAN, M.D.
General Surgery
Book an Appointment
-
![Prof. TAMER KARŞIDAĞ, M.D.]() Prof. TAMER KARŞIDAĞ, M.D.
General Surgery
Book an Appointment
Prof. TAMER KARŞIDAĞ, M.D.
General Surgery
Book an Appointment
-
![Prof. TANER KORKMAZ, M.D.]() Prof. TANER KORKMAZ, M.D.
Oncology
Book an Appointment
Prof. TANER KORKMAZ, M.D.
Oncology
Book an Appointment
-
![Assoc. Prof. A. ENES ARIKAN, M.D.]() Assoc. Prof. A. ENES ARIKAN, M.D.
General Surgery
Book an Appointment
Assoc. Prof. A. ENES ARIKAN, M.D.
General Surgery
Book an Appointment
-
![Assoc. Prof. DENİZ ATASOY, M.D.]() Assoc. Prof. DENİZ ATASOY, M.D.
General Surgery
Book an Appointment
Assoc. Prof. DENİZ ATASOY, M.D.
General Surgery
Book an Appointment
-
![Assoc. Prof. HALİL KARA, M.D.]() Assoc. Prof. HALİL KARA, M.D.
General Surgery
Book an Appointment
Assoc. Prof. HALİL KARA, M.D.
General Surgery
Book an Appointment
-
![Assoc. Prof. HAYRETTİN DİZEN, M.D.]() Assoc. Prof. HAYRETTİN DİZEN, M.D.
General Surgery
Book an Appointment
Assoc. Prof. HAYRETTİN DİZEN, M.D.
General Surgery
Book an Appointment
-
![Assoc. Prof. MURAT URKAN, M.D.]() Assoc. Prof. MURAT URKAN, M.D.
General Surgery
Book an Appointment
Assoc. Prof. MURAT URKAN, M.D.
General Surgery
Book an Appointment
-
![Assoc. Prof. ONUR DÜLGEROĞLU, M.D.]() Assoc. Prof. ONUR DÜLGEROĞLU, M.D.
General Surgery
Book an Appointment
Assoc. Prof. ONUR DÜLGEROĞLU, M.D.
General Surgery
Book an Appointment
-
![Assoc. Prof. ÖZDEN SILA ULUS BUTURAK, M.D.]() Assoc. Prof. ÖZDEN SILA ULUS BUTURAK, M.D.
Radiology
Book an Appointment
Assoc. Prof. ÖZDEN SILA ULUS BUTURAK, M.D.
Radiology
Book an Appointment
-
![AHMET ALAN, M.D.]() AHMET ALAN, M.D.
General Surgery
Book an Appointment
AHMET ALAN, M.D.
General Surgery
Book an Appointment
-
![ALİ ŞAHİN, M.D.]() ALİ ŞAHİN, M.D.
General Surgery
Book an Appointment
ALİ ŞAHİN, M.D.
General Surgery
Book an Appointment
-
![ALİ ŞENOL ÇELEBİ, M.D.]() ALİ ŞENOL ÇELEBİ, M.D.
Radiology
Book an Appointment
ALİ ŞENOL ÇELEBİ, M.D.
Radiology
Book an Appointment
-
![BİROL ESEN, M.D.]() BİROL ESEN, M.D.
General Surgery
Book an Appointment
BİROL ESEN, M.D.
General Surgery
Book an Appointment
-
![EMEL ÖZVERİ, M.D.]() EMEL ÖZVERİ, M.D.
General Surgery
Book an Appointment
EMEL ÖZVERİ, M.D.
General Surgery
Book an Appointment
-
![FAHRİ GÜVEN, M.D.]() FAHRİ GÜVEN, M.D.
General Surgery
Book an Appointment
FAHRİ GÜVEN, M.D.
General Surgery
Book an Appointment
-
![HÜSEYİN GÜNEY, M.D.]() HÜSEYİN GÜNEY, M.D.
General Surgery
Book an Appointment
HÜSEYİN GÜNEY, M.D.
General Surgery
Book an Appointment
-
![RAİF ORHAN, M.D.]() RAİF ORHAN, M.D.
General Surgery
Book an Appointment
RAİF ORHAN, M.D.
General Surgery
Book an Appointment
-
![SEDA ERDOĞDU, M.D.]() SEDA ERDOĞDU, M.D.
Radiation Oncology
Book an Appointment
SEDA ERDOĞDU, M.D.
Radiation Oncology
Book an Appointment
-
![SELİN ALPONAT, M.D.]() SELİN ALPONAT, M.D.
Pathology
Book an Appointment
SELİN ALPONAT, M.D.
Pathology
Book an Appointment
-
![TOLGA HÜNER, M.D.]() TOLGA HÜNER, M.D.
General Surgery
Book an Appointment
TOLGA HÜNER, M.D.
General Surgery
Book an Appointment
-
![ÜLKÜ TUBA PARLAKKILIÇ, M.D.]() ÜLKÜ TUBA PARLAKKILIÇ, M.D.
Radiology
Book an Appointment
ÜLKÜ TUBA PARLAKKILIÇ, M.D.
Radiology
Book an Appointment
-
![Clinical Psychologist EMİNE NAZ TANOĞLU, MSc]() Clinical Psychologist EMİNE NAZ TANOĞLU, MSc
Psychology
Book an Appointment
Clinical Psychologist EMİNE NAZ TANOĞLU, MSc
Psychology
Book an Appointment