Radiation Oncology Departments of Acıbadem Healthcare Group are units which examine effects of radiation on cancer and behaviors of tumors using ionizing radiation and conduct investigations in this field.
There are two practice areas in Radiation Oncology Departments of Acıbadem Healthcare Group; radiotherapy and radiosurgery.
Radiotherapy
Radiotherapy is defined as treatment of cancerous tissue and some benign tumors using radiation. Therefore, it is colloquially called “radiation therapy” or “X-ray therapy”.
Beams are used to prevent growth of cancerous cells or to kill them at the target of treatment. Radiotherapy is a commonly used treatment modality of cancer. In fact, radiotherapy may be required at least once in 60-80 percent of cancer patients, after diagnosis is made.
How is the treatment technique selected?
There are many factors that influence selection of the treatment method. Most important ones are patient’s age, overall health status, type of cancer, extent of metastasis and location. Treatment-related decisions are made with multidisciplinary approach, a process that requires examination of the patient by many specialists from multiple relevant medical departments.
A unique diagnostic and therapeutic plan is made and employed for each patient. Even if patients have same type of cancer, treatment should be planned according to patient-specific conditions.
Who is included in the therapy team?
Radiation Oncologist: A physician who decides how much radiotherapy will be applied to which part of body. This physician is responsible for following up the patient throughout the therapy, modifying the treatment depending on alterations in tumor and evaluating and managing side effects.
Radiation Physicist: These individuals are responsible for planning therapy and coordinating quality, safety and technical service as well as maintenance of devices. S/he works in collaboration with radiation oncologist in therapy planning and application.
Radiotherapy Technicians: These are the individuals who are trained to use radiotherapy devices. They do not stay with the patient in the same room during therapy; however, they are continuously in communication with the patient through a monitor found in the control room. They are responsible for positioning the patient correctly, operating the device and acquiring images for real time controls during therapy.
Oncology Nurse: s/he is member of team who stays most close to the patient, along with radiation oncologist, in treatment and follow-up of the patient. They act like a bridge between the physician and the patient to manage issues such as side effects and “Do’s and Don’ts”.
Secretariat: They are responsible for guiding the patient correctly, arranging appointments, creating and saving medical files, informing the patient about treatment expenses and performing procedures required by health insurance coverage of the patient.
What is Effect of Radiotherapy
Beams used in radiotherapy influence the DNA inside nucleus of tumor cells. These cells lose their ability to divide and grow when the DNA in nucleus is sufficiently damaged.
Since the destructed cells in cancerous tissue cannot reproduce, growth of cancer is ceased and size of tumor is reduced. High-dose radiation in a radiotherapy session either destroys the cells or hinders division. As tumor cells divide faster than most of the healthy cells, radiotherapy destroys these cells at higher rates. Although radiotherapy affects healthy cells in a certain extent, they can survive using special repair mechanisms which are not present in tumor cells.
Radiosurgery
Fundamental purpose of radiosurgery - an application field of radiation oncology - is creating changes in the diseased tissue by directing and focusing multiple low-energy beams towards the diseased area, resulting in delivery of high energy to the target zone. This way, it is ensured that cancer cells are reduced or destroyed in response to intensive beams delivered to the diseased area while nearby healthy tissues are protected against hazardous effects of radiation.
Radiosurgery Applications
STEREOTACTIC RADIOSURGERY (SRS)
SRS implies treating a target using certain coordinates; high-dose radiation destroys tumor completely in a single session, after coordinates are determined on three dimensional images. IGRT is critically important regarding actual destruction of the target in this procedure.
STEREOTACTIC RADIOTHERAPY (SRT)
SRT implies a treatment characterized by SRS given in more than one session, usually in 3 to 5 sessions.
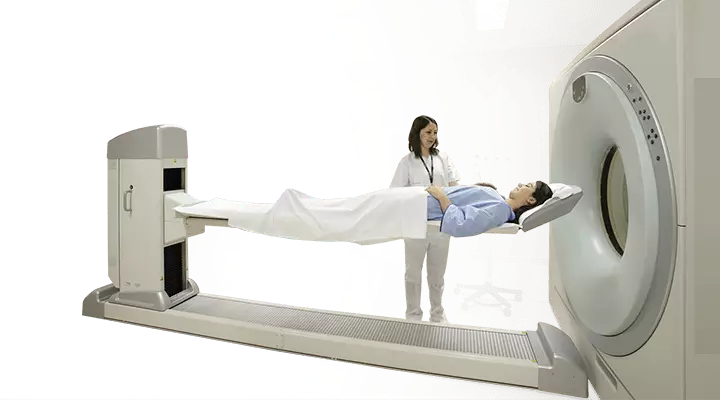
Medical devices such as MR-LINAC, Gamma Knife, TrueBeam, Tomotherapy, CyberKnife and Intra-operative Radiotherapy are used in Acıbadem Radiation Oncology Departments.
Doctors
-
![Prof. BÜNYAMİN KAPLAN, M.D.]() Prof. BÜNYAMİN KAPLAN, M.D.
Radiation Oncology
Prof. BÜNYAMİN KAPLAN, M.D.
Radiation Oncology
Book an Appointment
-
![Prof. ENİS ÖZYAR, M.D.]() Prof. ENİS ÖZYAR, M.D.
Radiation Oncology
Prof. ENİS ÖZYAR, M.D.
Radiation Oncology
Book an Appointment
-
![Prof. EVRİM KADRİYE TEZCANLI, M.D.]() Prof. EVRİM KADRİYE TEZCANLI, M.D.
Radiation Oncology
Prof. EVRİM KADRİYE TEZCANLI, M.D.
Radiation Oncology
Book an Appointment
-
![Prof. FULYA AĞAOĞLU, M.D.]() Prof. FULYA AĞAOĞLU, M.D.
Radiation Oncology
Prof. FULYA AĞAOĞLU, M.D.
Radiation Oncology
Book an Appointment
-
![Prof. GAMZE UĞURLUER SÜMER, M.D.]() Prof. GAMZE UĞURLUER SÜMER, M.D.
Radiation Oncology
Prof. GAMZE UĞURLUER SÜMER, M.D.
Radiation Oncology
Book an Appointment
-
![Prof. IŞIK ASLAY, M.D.]() Prof. IŞIK ASLAY, M.D.
Radiation Oncology
Prof. IŞIK ASLAY, M.D.
Radiation Oncology
Book an Appointment
-
![Prof. LÜTFİ ÖZKAN, M.D.]() Prof. LÜTFİ ÖZKAN, M.D.
Radiation Oncology
Prof. LÜTFİ ÖZKAN, M.D.
Radiation Oncology
Book an Appointment
-
![Prof. MEHMET UFUK ABACIOĞLU, M.D.]() Prof. MEHMET UFUK ABACIOĞLU, M.D.
Radiation Oncology
Prof. MEHMET UFUK ABACIOĞLU, M.D.
Radiation Oncology
Book an Appointment
-
![Prof. MELTEM SERİN, M.D.]() Prof. MELTEM SERİN, M.D.
Radiation Oncology
Prof. MELTEM SERİN, M.D.
Radiation Oncology
Book an Appointment
-
![Prof. MERİÇ ŞENGÖZ, M.D.]() Prof. MERİÇ ŞENGÖZ, M.D.
Radiation Oncology
Prof. MERİÇ ŞENGÖZ, M.D.
Radiation Oncology
Book an Appointment
-
 Prof. NEZİHE SEDEN KÜÇÜCÜK, M.D.
Radiation Oncology
Prof. NEZİHE SEDEN KÜÇÜCÜK, M.D.
Radiation Oncology
Book an Appointment
-
![Prof. NURAN BEŞE, M.D.]() Prof. NURAN BEŞE, M.D.
Radiation Oncology
Prof. NURAN BEŞE, M.D.
Radiation Oncology
Book an Appointment
-
![Assoc. Prof. FUZULİ TUĞRUL, M.D.]() Assoc. Prof. FUZULİ TUĞRUL, M.D.
Radiation Oncology
Assoc. Prof. FUZULİ TUĞRUL, M.D.
Radiation Oncology
Book an Appointment
-
![Assoc. Prof. SERAP YÜCEL, M.D.]() Assoc. Prof. SERAP YÜCEL, M.D.
Radiation Oncology
Assoc. Prof. SERAP YÜCEL, M.D.
Radiation Oncology
Book an Appointment
-
![ALPTEKİN ARİFOĞLU, M.D.]() ALPTEKİN ARİFOĞLU, M.D.
Radiation Oncology
ALPTEKİN ARİFOĞLU, M.D.
Radiation Oncology
Book an Appointment
-
![ASLI SARAN İKİZLER, M.D.]() ASLI SARAN İKİZLER, M.D.
Radiation Oncology
ASLI SARAN İKİZLER, M.D.
Radiation Oncology
Book an Appointment
-
![BURCU DURMAK İŞMAN, M.D.]() BURCU DURMAK İŞMAN, M.D.
Radiation Oncology
BURCU DURMAK İŞMAN, M.D.
Radiation Oncology
Book an Appointment
-
![ERTUĞRUL TEKÇE, M.D.]() ERTUĞRUL TEKÇE, M.D.
Radiation Oncology
ERTUĞRUL TEKÇE, M.D.
Radiation Oncology
Book an Appointment
-
![KADİR UÇAR, M.D.]() KADİR UÇAR, M.D.
Radiation Oncology
KADİR UÇAR, M.D.
Radiation Oncology
Book an Appointment
-
![LEYLA ŞEN, M.D.]() LEYLA ŞEN, M.D.
Radiation Oncology
LEYLA ŞEN, M.D.
Radiation Oncology
Book an Appointment
-
![OSMAN BURAK CAN, M.D.]() OSMAN BURAK CAN, M.D.
Radiation Oncology
OSMAN BURAK CAN, M.D.
Radiation Oncology
Book an Appointment
-
![SEDA ERDOĞDU, M.D.]() SEDA ERDOĞDU, M.D.
Radiation Oncology
SEDA ERDOĞDU, M.D.
Radiation Oncology
Book an Appointment
-
![SEDENAY OSKEROĞLU KAPLAN, M.D.]() SEDENAY OSKEROĞLU KAPLAN, M.D.
Radiation Oncology
SEDENAY OSKEROĞLU KAPLAN, M.D.
Radiation Oncology
Book an Appointment
-
![ZEYNEP GÜRAL, M.D.]() ZEYNEP GÜRAL, M.D.
Radiation Oncology
ZEYNEP GÜRAL, M.D.
Radiation Oncology
Book an Appointment
Medical Technologies
Hospitals
-
![Adana Hospital]() Adana Hospital
Adana Hospital -
![Altunizade Hospital]() Altunizade Hospital
Altunizade Hospital -
![Atakent Hospital]() Atakent Hospital
Atakent Hospital -
![Ataşehir Hospital]() Ataşehir Hospital
Ataşehir Hospital -
![Bodrum Hospital]() Bodrum Hospital
Bodrum Hospital -
![Bursa Hospital]() Bursa Hospital
Bursa Hospital -
![Eskişehir Hospital]() Eskişehir Hospital
Eskişehir Hospital -
![İzmir Kent Hospital]() İzmir Kent Hospital
İzmir Kent Hospital -
![Kayseri Hospital]() Kayseri Hospital
Kayseri Hospital -
![Maslak Hospital]() Maslak Hospital
Maslak Hospital